SURGICAL CAMPAIGN AT KINGTOM POLICE HOSPITAL IN FREETOWN, SIERRA LEONE.

DATE: 14-23 NOVEMBER 2025
The team began to form in April and was complete in June with 11 people (anaesthesia, nursing, general surgery and paediatric surgery). The campaign took place between 14 and 23 November.
DOCUMENTATION AND VISAS:
To travel to Sierra Leone, the only mandatory documentation is a valid passport, with a minimum validity of 6 months from the date of entry, a visa and a yellow fever vaccination certificate.
The visa is an electronic visa (E-Visa) that is very easy to obtain. You just have to apply online (https://www.evisa.sl/#/home) and pay the fee (84.27 USD, 80 for the visa and 4.27 for processing costs). The yellow fever vaccination certificate is an official certificate that is obtained after receiving the vaccine and paying a fee (currently €19.46). It is advisable to visit one of the authorised international vaccination centres at least one month before departure. A list of these centres can be found on the Ministry of Health website (https://www.sanidad.gob.es/areas/sanidadExterior/laSaludTambienViaja/centrosVacunacionInternacio nal/centrosvacu.htm).
In addition, it is advisable to take out travel insurance and professional liability insurance. The Foundation for International Cooperation of the Medical Association (https://www.fcomci.com) offers liability and travel insurance for registered doctors who are listed in the national register of cooperating doctors of that organisation. Some nursing associations, such as the one in Madrid, have taken out civil liability insurance for their members that includes humanitarian aid activities. Some individually taken out insurance policies can also be temporarily extended to cover international cooperation abroad.
In addition, a series of documents must be processed for temporary work permits in Sierra Leone, which are: a certified translation into English of the degree (bachelor’s degree or specialisation for doctors and diploma/degree for nurses), a summary CV in English, a certificate of professional suitability/certificate of good conduct (which can be requested from the official associations), and a registration form for the Medical and Dental Council of Sierra Leone (the latter only for doctors). Apart from the cost of the certified translation, if you do not already have one, and the fee for the certificate of professional suitability charged by some professional associations, the procedure is free of charge.
TRANSPORT:

The flights were arranged from Madrid with the help of Angelis González, a freelance travel agent with Halcón Viajes, which has been collaborating with the Cirujanos en Acción Foundation for years.
The five team members who came from outside Madrid (one from Segovia, one from Menorca, one from Murcia and two from Lleida) arranged their own travel to Madrid.
The team travelled on Thursday, 13 November 2025, at 7:00 p.m. from Madrid to Freetown with a three-hour stopover in Casablanca, arriving at Lungi Airport in Freetown on 14 November 2025 at 3:35 a.m.
The return journey took place on Sunday 23/11/2025 at 6:50 a.m., with the trip beginning at 2:00 a.m. to reach the airport by ferry. There was also a stopover, this time of two hours, in Casablanca, arriving in Madrid at 3:30 p.m.
These flights with Royal Air Maroc were chosen because they allowed us to travel more quickly and their dates were more convenient for the campaign, despite some bad experiences with lost luggage.
Indeed, five of the packages did not arrive in Freetown initially. After filing the corresponding claims at Lungi Airport and taking the necessary steps, both by Dr Konteh from Sierra Leone and by Angelis González and David Luengas from Madrid, three of the five lost packages were located and arrived in Freetown on 21 November (the last day of the campaign). The other two packages arrived, without prior notice, on 27 November, when the team was already back in Spain. It was agreed with John Konteh that they would be kept for the next campaign, which will take place in January.
For internal transport, airport police personnel were waiting for us on arrival to help us speed up border formalities and, once through customs, we were met by Dr John Konteh, Deputy Director and Medical Superintendent of the Sierra Leone Police Medical Services, who was our contact person prior to arrival to organize everything necessary. He accompanied us to take the Seacoach Express.
This is a ferry that connects the airport (located in Lungi Town) with the Freetown peninsula, and is the fastest way to get there, as ground transportation involves a 3-hour trip around Tagrin Bay. The price is
$45 per person per trip and includes the shuttle bus from the airport to the ferry terminal (about 5-10 minutes) and the ferry ride, which takes about 45 minutes.
From the Freetown ferry terminal, we travelled to the hotel in a Toyota Coaster minibus with official police registration plates, which took us daily from the hotel to the hospital and back.
We also used it for the trips we made on our last day, which was a day off.
TRANSFER OF MATERIAL:
A total of 22 pieces of checked luggage weighing between 18 and 23 kg were transported, containing surgical and anaesthetic equipment, including two anaesthesia monitors loaned to one of the anaesthetists (Celia Garrido) and two electric scalpel generators belonging to the foundation.
The team was responsible for obtaining the necessary materials for the campaign.
The 12 de Octubre Hospital in Madrid donated anaesthetic medication worth €750, arranged by anaesthetist Javier Silva.
We also received a donation of sutures worth €1,000 from B Braun, arranged by paediatric surgeon Rocío Gutiérrez.
A fellow general surgeon from 12 de Octubre Hospital, Alfredo Vivas, who did not attend the campaign but wanted to collaborate, made a personal donation of 25 boxes of 40 1g paracetamol tablets and 15 200ml bottles of ibuprofen syrup (20mg/ml), enough to provide post-operative analgesia for all patients who underwent surgery.
The surgical meshes used were fragments of polypropylene meshes cut under sterile conditions and subsequently re-sterilized at the 12 de Octubre Hospital.
The rest of the material (surgical gowns, sterile cloths, gauze, compresses, sutures, dressings, gloves, antiseptic solutions, electric scalpel terminals and plates, scalpel blades, anaesthetic medication, syringes, needles, IV lines, etc.) were obtained as part of small donations from the hospitals where all the participants work, and some material was also taken from the warehouse of the Cirujanos en Acción foundation.
ACCOMMODATION:
As in previous campaigns, we stayed at the Jam Lodge Hotel. The hotel is quiet and offers single or double rooms with private bathrooms and breakfast included in the price. It is also located about 10-15 minutes from the hospital, which makes it convenient for starting and ending the day. As with the last group in September, we made the reservation through Booking, as it was cheaper than booking directly with the hotel. And thanks to the Genius discounts of one of the team members (Nacho Ortega), who made all the reservations, we got a discount of up to 32% off the original price, so the price for 8 nights for single rooms was £375.12 and for double rooms £515.92. To that we had to add a total of £70 per room to be allowed to check in early on the day of arrival (we arrived around 7:30 a.m. and check-in time is 3:00 p.m.) and a late check-out on the day of departure (we kept the room until 7:30 p.m.).

ADULT PATIENTS
A total of 137 procedures were performed on 116 patients.
PEDIATRIC PATIENTS
A total of 62 procedures were performed on 57 patients.
According to local staff, no complications were reported either during the campaign or afterwards.
1. CAMPAIGN REPORT
2.1. THE LOCATION
Freetown, the capital of Sierra Leone, is a destination where the Cirujanos en Acción Foundation has established ties since 2019, when the first surgical campaign was carried out in this city in this West African country.
The health center where the campaign took place was the Kingtom Police Hospital in Freetown, a facility belonging to the police force, an institution with considerable influence and power throughout the country. In the past, this hospital only treated members of the police force and their families, but in recent years it has extended its medical services to the entire population of the area.
The hospital consists of several modules for emergency care, basic primary care, obstetrics consultations, etc.
The module where the surgical block is located has two floors. On the upper floor, there are several hospital rooms, offices, and consultation rooms.
It has a basic laboratory (simple blood counts and biochemistry, basic urine analysis and rapid tests for various pathologies, including HIV).
The surgical area is located on the ground floor. It has two operating theatres (one large and one small), separated by the sterilization room with an autoclave and a small room with a sink, all connected.

Adjacent to the large operating theatre is a small room with a table where we were brought coffee and fruit and ate lunch. Adjacent to the small operating theatre is a room with cupboards and a bathroom that we used to store the equipment we brought with us. On the first floor, we were given another room with a bathroom and a key, which we used as a changing room and to leave our personal belongings.
Both operating theatres have air conditioning, although it did not always work properly.
Outside the surgical area on the same floor, there are three hospital rooms that were used during the campaign for surgical patients (one for men, one for women and one for children).
There are also two offices (one of them belonging to John Konteh) that we use as consultation rooms on the first day to carry out triage.
2.2. THE TEAM
Our team consisted of a total of 11 volunteers:
- Nursing: Carlota Castillo Sainz, Assumpta Ferrer Benejam and Laia Ribelles Moreno.
- Paediatric Surgery: Rocío Soledad Gutiérrez and Detlef Oliu San Miguel.
- General Surgery: Sandra del Barrio Anaya, Marta Gutiérrez Andreu, Ignacio Ortega Fernández and Daniel Pastor Altaba (team leader).
- Anaesthesia: Celia Garrido Yuste and Javier Silva García.
2.3. LOCAL STAFF

Dr John Konteh, Deputy Director and Medical Superintendent of the Sierra Leone Police Medical Services, is, as mentioned above, the contact person responsible for coordinating the campaign with us. He is a highly experienced endocrinologist who trained in London, which enables him to understand our point of view very easily. He is responsible for organizing all local transport and making preliminary calls to patients for the campaign, based on what has been agreed (in our case, we agreed that we would perform paediatric and adult surgery, but not endocrine surgery, and he was responsible for gathering more than 400 patients who were candidates for surgery).
Although he was not present in the surgical area, he was present at the hospital on many occasions and available by telephone at all times.
In addition, we had the enormous support of David Fanday, the hospital’s nursing administrator, who was always looking out for us and accompanied us on our trips from the hotel to the hospital and vice versa. Furthermore, given that five of the packages were missing, and that one of them contained almost half of the anaesthetic medication and all of the spinal anaesthesia needles, we had to obtain supplies locally in order to carry out the campaign. Thanks to David and Dr Konteh, we were able to obtain everything we needed on a daily basis to continue with the surgical activity. It was thanks to them and the enormous adaptability of the anaesthetists, especially Javier Silva, who was in charge of the two adult tables, that the campaign was able to go ahead.
However, we must also mention and thank the rest of the staff who were present and collaborating during the long surgical days (Mohamed Sorie Kamara, Unisa Sesay, Francis Raymond Kamara, Mary T. Musa, Bintu Jimmisa, Davida Dumbuya, Fatmata Kabba, Francis S. Conteh, Philipp Kpange…), the nursing staff who were responsible for calling the patients who had to come in each day, preparing them before surgery, caring for them in the immediate post-operative period, collaborating with us in the operations and being in charge of cleaning and re-sterilizing materials.
On some days, we had the help of Sia, an anaesthesia technician who works at the Italian hospital but who came to help with the campaign at the Police Hospital when he was available.
We were also accompanied by some nursing students (Sheriff, Ibrahim, Konneh…) who were very committed and eager to learn.
2.4. EQUIPMENT
The hospital has acceptable surgical equipment for minor surgeries (inguinal hernias, soft tissue tumors, small ventral hernias, etc.), which is the type of surgery we perform. Some of the equipment is already very worn (Kocher clamps that do not close properly or needle holders that do not grip the needle well, for example), but it can still be used for these types of procedures. There is enough to prepare several boxes with two toothed forceps, two non-toothed forceps, needle holders, mosquito forceps, Kocher forceps, scissors and retractors, and to re-sterilize without having to wait. For more complex or delicate surgery such as thyroidectomies, I think it is advisable to bring your own equipment. In our case, Rocío Gutiérrez, a paediatric surgeon, brought a couple of boxes of instruments that were used for paediatric cases.
There is an electric scalpel that also works “acceptably” (increasing the power significantly to be able to coagulate), with a metal plate but compatible with the adhesive plates we normally use here, and with a three-prong connector for the button terminal. We brought two more generators, so we had one per table. In Sierra Leone, the mains voltage is 230V and the frequency is 50Hz, and the power socket is type G (British). It is important to remember to bring adapters so that the earth connection works properly. As for consumables, it is best to bring them from Spain. However, since five of our packages were lost and we only recovered three on the last day, we ran out of gowns and gauze during the last few days.
There are cloth gowns that can be re-sterilized, and gauze can also be obtained there.
As for lighting, there are only two large lights, one of which broke on the first day and could not be repaired while we were there. There are a couple of smaller lights that are not very mobile and are completely insufficient. Therefore, a good-quality head torch is essential (torches with built-in batteries tend to give off little light. It is better to use one with replaceable batteries, which are usually more powerful and also allow you to have spare batteries, as surgical procedures are long and the batteries start to fail in the last few hours, when the light is most needed).
2.5. ANAESTHESIA
There is currently a Dräger Atlan ventilator with Isoflurane and Sevoflurane vaporizers (donated by the Bisturí Solidario foundation) installed in the larger operating theatre. The installation consists of an oxygen connection connected via a tube to a replaceable O2 cylinder and a medical air generator to mix the gases. The dependence on an oxygen cylinder limits the use of high flows and inhalation inductions, as it is consumed at a faster rate, but most paediatric patients had an intravenous line, which allowed for intravenous inductions.
Our initial intention was to use the smaller operating theatre for paediatric patients and the larger one for two adult tables. However, although it would have been feasible to move the anaesthesia machine, as the only “fixed” element is the oxygen hose, which is anchored to the wall with clamps, we did not risk moving the ventilator, which had caused problems in previous campaigns and was working well in our campaign. Therefore, we set up one paediatric table and one adult table in the large operating theatre and another adult table in the small one.
There is another ventilator outside the operating theatre that had previously been working but was awaiting repair.
There are also three oxygen concentrators, although only two were working and at times they had problems due to power failures.
The anaesthesia machine has a multi-parameter monitor, but some of the measurements were not available, so it was necessary to supplement it with portable pulse oximeters. The machine’s ventilator has capnography. Each adult table has a Phillips mp monitor that allows complete monitoring, although at times it was necessary to use them on battery power due to the limited number of working sockets, which meant that they shut down at certain times. One of them had a problem measuring blood pressure. In these cases, a portable blood pressure monitor owned by the hospital and small portable pulse oximeters carried by the team were used.
Adults:
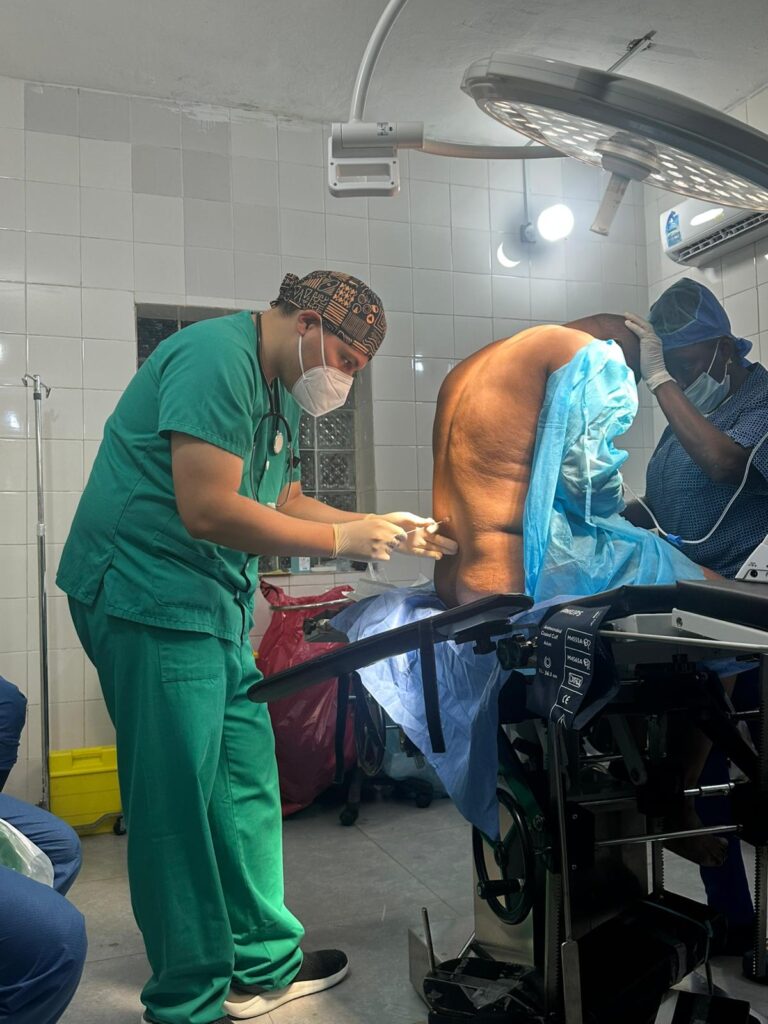
As there was only one anaesthesia machine in operation, it was used for paediatric patients, and almost all adults underwent spinal or local anaesthesia combined with more or less deep sedation when necessary, mainly combining propofol and ketamine in spontaneous breathing with nasal cannulas and, in some cases, clearing the airway with Guedel-type cannulas when deeper anaesthesia was required. In this regard, it should be noted that the soft tissue injuries were large, and almost all required moderate to deep sedation given the limitation in achieving an adequate level of anaesthesia using only local anaesthesia.
It should also be noted that the performance of intrathecal anaesthesia was conditioned by the lack of intrathecal needles due to the loss of luggage, so different models from other campaigns and those that could be obtained from the hospital were used. From an anatomical point of view, ligaments in general are highly resistant, and the dosage tends to be higher given the younger age of the population and greater body size compared to our population (doses between 13-17 mg of hyperbaric bupivacaine depending on the location of the intervention area), with adequate tolerance.
Haemodynamics. On the first day, we observed a lack of effect from the hyperbaric bupivacaine used, which was resolved by changing batches, without being able to establish the cause. We do not know whether temperature changes during transport can alter the medication. Given the limited supplies, the packaging of sterile gloves was used as a sterile field for the intradural technique, and cloths were not used to delimit the puncture field, replacing it with extensive cleaning of the entire back and hips with alcoholic chlorhexidine. In general, local anaesthesia was not administered prior to intradural puncture for the same reason, so punctures were generally performed with intradural needles without an introducer.
Locally, intravenous catheters with ports for administering medication, infusion lines, and 0.9% saline solution are available without restrictions, which allowed all patients to be hydrated before the intradural procedure. It should be noted that patients undergo prolonged fasting and that heat and humidity are significant factors. The lines were cannulated by local staff before transfer to the operating theatre, but it is advisable to check them thoroughly before use, as a percentage of them were extravasated.
Only one case was performed under general anaesthesia, which had been impossible to anaesthetise regionally a few days earlier and was rescheduled for the last day when the paediatric cases were completed. No allergic reactions were recorded, only four patients presented hypotension after anaesthetic induction, which was resolved with the timely administration of ephedrine, and one episode of vasovagal presyncope due to pain during a procedure under local anaesthesia, which was resolved with atropine and conversion to deep sedation. Once again, we emphasize the importance of monitoring and administering anxiolysis and/or sedation in procedures proposed for local anaesthesia.
Paediatrics:
All procedures were performed under general anaesthesia with a laryngeal mask, either with sevoflurane (a vaporizer and limited supply of the agent are available) or with intravenous bolus maintenance (no infusion pump is available). The use of inhalation anaesthesia is limited by the consumption generated by the inability to perform low flows and by the consumption of oxygen cylinders. In some cases where the oxygen cylinder was depleted during the procedure, it was necessary to switch to an oxygen concentrator via a Mapleson mask in spontaneous ventilation. All paediatric patients received local anaesthesia to reduce anaesthetic requirements given the lack of fentanyl and limited ketamine due to lost luggage.
Most of the children had a venous line prior to the procedure, which facilitated intravenous induction. There was only one case of severe laryngospasm/bronchospasm and loss of venous access with difficulty in recanalization.
To be taken into account in the next campaign, the suitcase that arrived later contained numerous intrathecal needles, most of which have an NRFit connection, requiring syringes with the same connection, which are transported in the same package. This limits the use of these syringes for intravenous drugs and vice versa, so we recommend bringing a large supply of syringes for administering medication, as there are no infusion pumps either.
2.6. ASEPTIC TECHNIQUES AND SURGICAL EQUIPMENT
There is a steam autoclave that allows the material to be re-sterilized (in metal trays and double cloth). Gowns, cloths and gauze can also be sterilized. We also re-sterilize electric scalpel tips, which generally last for 2-3 uses before eventually ceasing to function. The local staff carry out the cleaning and re- sterilization tasks very efficiently and we had no problems in this regard.
2.7. OUR LIFE IN FREETOWN
We arrived at Freetown International Airport in Lungi Town on Friday, 14 November 2025, at 4:30 a.m. After retrieving the 17 pieces of luggage (out of a total of 22 checked) that had arrived and filing the corresponding claims for the lost luggage, we passed through customs. John Konteh met us in the arrivals area, and together we took the ferry and then the minibus to the hotel, arriving between 7:30 and 8:00 am.
After resting for a few hours, at 12 noon we were picked up and taken to the hospital, where we were greeted by the local team and hundreds of patients waiting to be triaged.
After opening the packages that had arrived, to get an idea of what was missing and what we could start operating on in the first few days, the surgeons began to consult with the patients while anaesthetists and nurses set up the equipment and organized the operating theatre area. After triaging some 230 patients and informing them that not all of them could probably be operated on, we decided to stop, even though there were still more than 100 patients waiting.
That day we had dinner at the hotel (we had ordered dinner in advance) for $15 per person. From Saturday 15/11/2025 to Friday 21/11/2025 we performed surgical procedures.
We had breakfast every day at the hotel around 7:00 a.m., and at 7:30 a.m. David, Abu (John Konteh’s personal bodyguard who accompanied us the entire time), and the driver picked us up in the bus. The trip to the hospital took about 10-15 minutes (depending on traffic, although we were often escorted by a police motorcycle that cleared the traffic ahead of us).
We started work at around 8:00 a.m. While the surgeons checked on the patients who had undergone surgery the previous day, the rest of us organized the operating theatres to begin surgical activity, with three tables (two for adults and one for children). Between 2:30 and 3:00 p.m., we all took a break to eat. The first few days, they brought us fruit and bread, and we ate cold cuts that we had brought from Spain, but the last few days we ordered local food (for 50 leones per person (less than 2 euros), they brought us rice with potato leaves or cassava and meat or fish. We also had fried plantains if we ordered them first thing in the morning (paying for them separately). There isn’t much variety, but it’s local food, and although it can get tiresome if you have it every day, it’s fine for a few days.

Then we continued until we finished with the patients scheduled for the day. We usually finished between 8:00 p.m. and 9:00 p.m.
For dinner, we only ordered dinner at the hotel on the first day. The rest of the days, we ordered dinner from a restaurant near the hotel and the hospital (with the help of David, who was always available) and picked it up on the way back to the hotel at the end of the day (chicken, salads, meat, pizza). Several days we decided to eat directly at the restaurant, inviting David, Abu, and the driver.
On Monday, 17 November 2025, we started a little later because, as every year, we were received first thing in the morning by the Inspector General of the Sierra Leone Police (Mr. William Faya Sellu) at a formal ceremony in which both he and Dr. John Konteh thanked the team and Cirujanos en Acción for their work at the Police Hospital in recent years, and we were given our temporary work permits.
On the last day of work, Friday 21/11/2025, we finished early in the afternoon so that we could rest a little more that day.
On Saturday, 22 November 2025, we took the day off. In the morning, we visited the Tacugama chimpanzee sanctuary, which is about 40 minutes from the hotel (we had the police bus and the company of David and Abu for transport on this day). This center is responsible for rehabilitating rescued chimpanzees (most of which had been sold as pets) so that they can return to their natural environment. The visit costs 350 leones (about £13) and lasts approximately one hour.

Then we visited the Cotton Tree (national symbol) and a craft market.
After resting for a while at the hotel, we were picked up at around 7:00 p.m., with all our luggage, to go to the official farewell dinner with the hospital staff, where we were also given some gifts. After dinner and a few hours of partying, we went straight to the ferry terminal to catch the ferry to the airport and catch our flight on Sunday 23/11/2025 at 6:50 am.
2. CONCLUSION
2.1 Strengths of this place:
The hospital’s appeal is so great that patients from neighbor countries have also been attending recent campaigns, which helps Cirujanos en Acción reach a larger number of people. Working hand in hand with the police makes any kind of administrative task much easier (there were no problems at customs on arrival despite transporting large quantities of surgical equipment and medicines, we were not stopped at any roadblocks and even during peak traffic hours we got through without any problems). Furthermore, as the campaign is in Freetown, there is no need for long internal journeys after arrival. Another advantage is that, in cases of lost luggage, as happened to us, it has been possible to obtain replacement materials (which would have been much more difficult, if not impossible, had we been in a more isolated area).
The local team has always been very involved and helpful at all times. They also take advantage of the campaigns to bring in nursing students as a training opportunity.
All of this has made for a very pleasant working environment.
3.2. Areas for improvement:
Although conditions in the surgical area have improved over time (new fan, air conditioning in almost all rooms, adequate sterilization capacity, etc.), there are still areas for improvement. The lights are not of good quality and are insufficient for the three tables, making a head torch essential for safe operation. The surgical equipment, although sufficient in quantity for minor surgeries, is not of very good quality. The operating tables are also old and sometimes do not maintain their position (the height gradually lowers).
The ventilator, although new, is connected to an oxygen cylinder, which prevents it from being used to its full capacity.
It would also be useful to have another ventilator in the second operating theatre.
Nevertheless, this hospital more than meets the expectations for surgical campaigns, and conditions will likely continue to improve over time.
3. BUDGET: (brief breakdown of expenses)
4.1. COST PER PARTICIPANT:
Flights: €1,085
Visa: 84.27 USDà 72 euros Luggage transport (packaging): €20
Ferry: 70 USD (35 per trip)à 60 euros
Accommodation: USD 670 double room (335 per person). USD 530 single room (average of USD 450 USD)à572 euros double (286 per person), 452 euros single (average, 361.5 euros) Meals (lunch, dinner and beers): 104.53 euros
Total price per person: Between €1,630 and €1,795 per person approximately (depending on whether you share a room or not).
4.2. TOTAL COST OF THE CAMPAIGN:
Total cost for the 11 participants, including flights, visas, transport, accommodation and living expenses:
€18,755 in total.
4. SIGNATURES
Signed on behalf of the entire team: Daniel Pastor Altaba, team leader. Surgeons in Action
PASTOR ALTABA