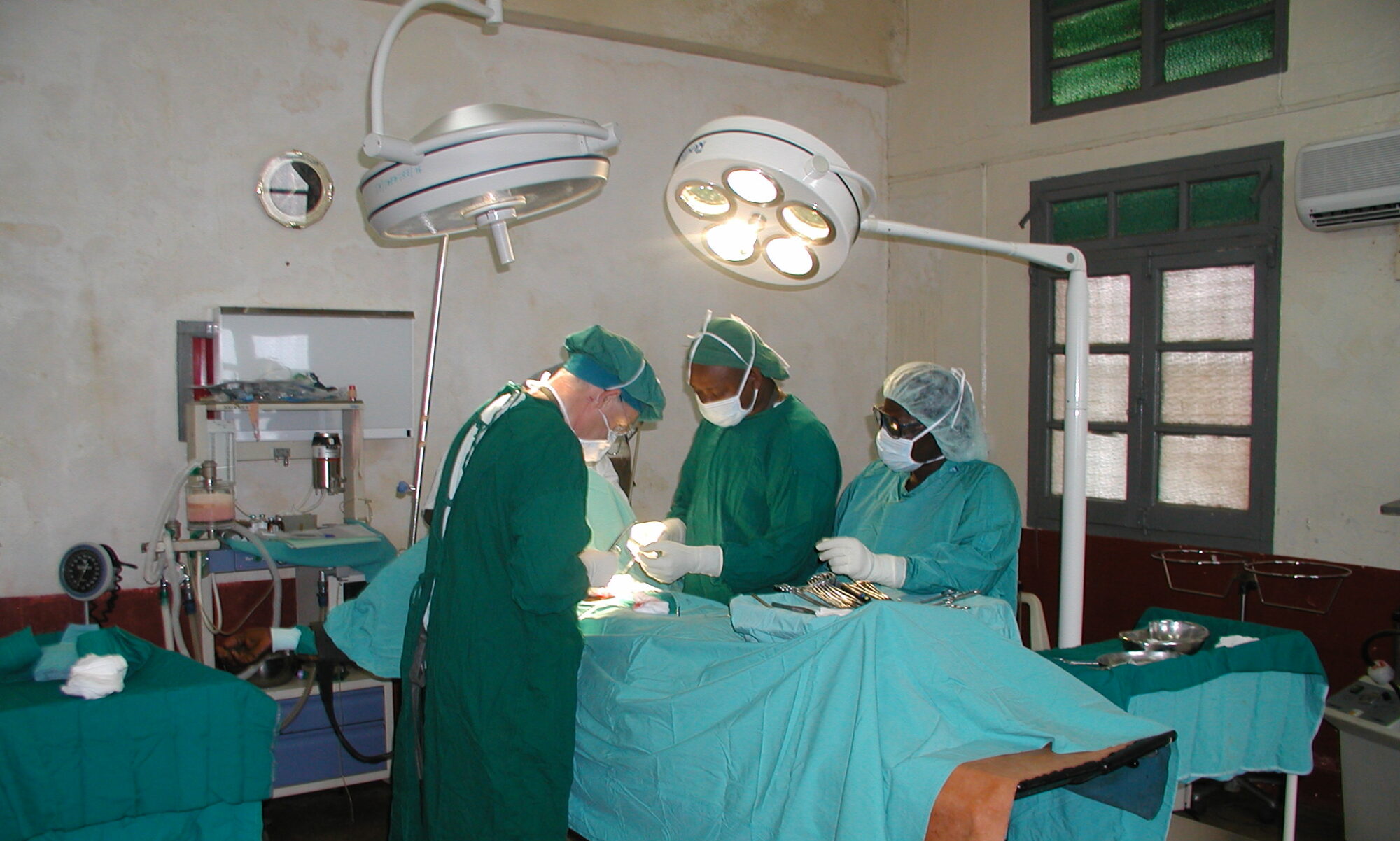
HERNIA INTERNATIONAL CAMPAIGN REPORT – KISOGA, MUKONO (UGANDA)
19–25 October 2025
Introduction
In April 2025, the opportunity arose to organise a new surgical campaign in Uganda, specifically at the Herona Community Hospital. The proposal was initially made by Professor Andrew Kingsnorth to Dr Teresa Butrón (Cirujanos en Acción).
Our usual cooperation group, without a fixed destination for this year, proposed to take on the organisation of the mission and began contacting volunteers willing to participate.

The final dates were set for 19–25 October 2025, and the team was composed of two female surgeons, three male surgeons, one urology resident, two anaesthetists, and one nurse. Most of the team members had previously taken part in other missions and had substantial experience in surgical cooperation.
Background
People living in rural areas of Africa often face a lack of immediate or specialised medical care. Life in these regions is economically difficult, with many people surviving on less than one US dollar per day. The lack of adequate medical resources exacerbates diseases such as malaria, HIV/AIDS, and maternal and child health issues. In Sub-Saharan Africa, more than six million underprivileged patients suffer from untreated hernias.
In Uganda, the Mukono District is a typical example of this problem. Covering an area of more than 1,875 square kilometres with a population exceeding 800,000 and growing at an annual rate of 2.7%, the district’s public hospitals and clinics are poorly equipped and lack even basic medicines. Patients with more severe conditions often must travel between 50 and 100 kilometres along rough roads to reach better-equipped hospitals in Kampala or Naggalama.



Recent improvements to the road leading to Kioga have opened the district and facilitated transport, but with a negative side effect: an increase in serious road accidents requiring emergency and life-saving surgical care, which is not locally available.

Destination
Our mission, carried out in cooperation with the Hernia International Charity, was based at Herona Community Hospital in Kisoga, Mukono District, Uganda. The hospital’s founder is Dr Mukalazi Henry Garvin, who, through great personal effort, has provided healthcare services to the population of Kisoga and surrounding areas with the following objectives:
- To provide medical and diagnostic imaging services
- To reduce maternal and child morbidity and mortality
- To offer comprehensive HIV care and reduce related morbidity and mortality
- To provide basic dental care, such as extractions
- To carry out child vaccination campaigns
- To perform minor surgical procedures
- To operate a basic diagnostic laboratory
The Region: Kisoga and Mukono District
Kisoga is a town located in the Mukono District, one of Uganda’s administrative divisions in the country’s central region. Like most other districts, its name derives from its capital, the town of Mukono, with a population of about 162,000 people. The district is notable for the Mabira Forest and its proximity to Lake Victoria. The total area is approximately 11,764 km² with a population of around 808,000 inhabitants, giving a population density of 69 people per square kilometre.

Herona Community Hospital
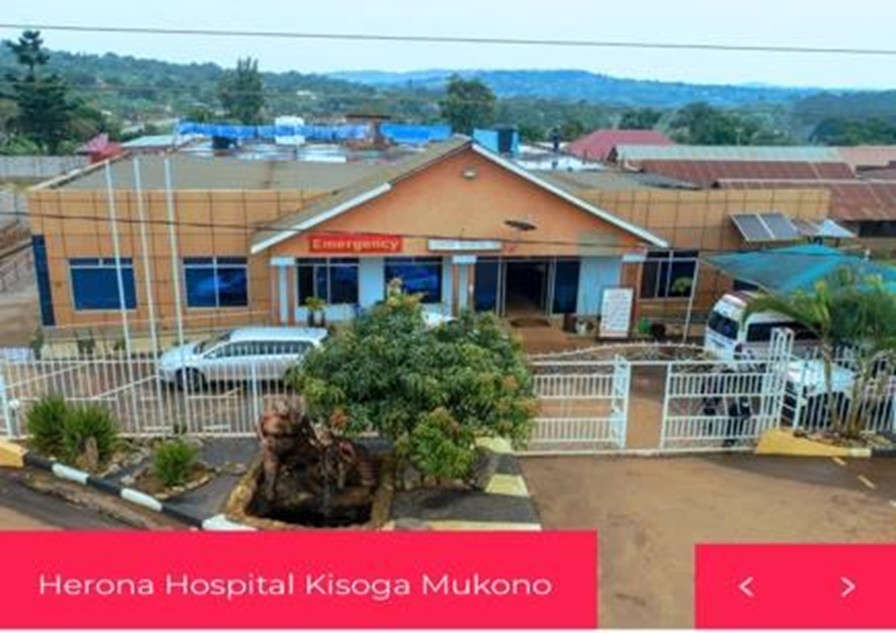
The Herona Community Hospital is a healthcare institution located in Kisoga, approximately 85 km from Entebbe International Airport.
In 2013, Dr Mukalazi Henry Garvin, born in Kisoga, decided to create a diagnostic imaging centre in his hometown, founding the Herona Medical and Imaging Centre as a private, non-profit entity registered and licensed by the Ugandan Ministry of Health. His goal was to provide affordable healthcare services to the local community, particularly in the sub counties of Kisoga and Ntenjeru, six neighbouring counties, and Koome Island on Lake Victoria, about 12 km to the south.


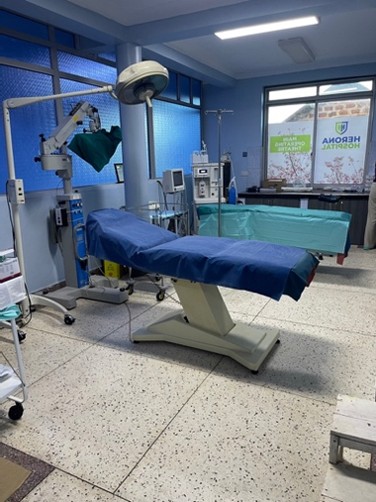
The hospital, with a capacity of about 50 beds, offers a range of medical services, including general consultations, maternity services, and minor surgery. It has a surgical area with two separate operating rooms, allowing us to operate on three surgical tables simultaneously.
Equipment and Facilities
The surgical area has two operating rooms; in one of them, we set up two surgical tables, though there were no overhead lights or general anaesthesia equipment. One electrosurgical unit failed on the first day, but this was solved thanks to a new unit we had transported from Spain, donated by the Fundació Antonius Musa of the Col·legi de Metges de Tarragona. The other operating room had one surgical table, overhead lighting, an electrosurgical unit, and a general anaesthesia machine.

Adjacent to this area is the sterilisation room, equipped with an-autoclave donated by Hernia International on a recent visit to the hospital by Professor Andrew Kingsnorth, a few weeks earlier to ensure its correct operation.
The hospital also includes wards for adults and children on the same floor as the operating area, a waiting area, an emergency room, and consultation rooms near the entrance. The radiology room, currently unequipped, was used as our dining room for lunch. There is also a large garden, where on Sunday afternoon we held the team’s presentation to the patients and their families before conducting examinations and scheduling surgeries.

The Team
The logistics for a surgical cooperation mission begin months in advance, starting with the voluntary selection of team members. Experience in abdominal wall pathology is highly valued, but participants must also be able to take time off and cover their own expenses, including flights, transport, accommodation, and meals.

Spanish Team – Kisoga, Uganda 2025
Campaign Coordinator:
Francesc Marsal Cavallé, Surgeon. Tarragona
Team Leader:
María del Pilar Concejo Cutolí, Surgeon. Valladolid
Team Members:
- Rosario Pérez Huertas, Surgeon. Sevilla
- Mar Felipe Correoso, Anaesthetist. Barcelona
- Meritxell Ojer Catalán, Anaesthetist. Barcelona
- Enric Caubet Busquet, Surgeon. Barcelona
- Mercè Oller Codina, Nurse. Barcelona
- Rosario Rodríguez Pérez, Urology Resident. Sevilla
- Antonio Javier Tejada Gómez, Surgeon. Sevilla
Local Team
The local director and coordinator of the entire campaign was Dr Mukalazi Henry Garvin.
The theatre assistants, Fred and Pius, were responsible for transferring instruments and handling washing and sterilisation. Viola and Jane are the nurses. Two surgical residents, Swaid and Isaac, participated actively in the operations, and Musa oversaw the ward.
We were impressed by the professionalism and cooperation of all hospital staff, as well as by Dr Garvin’s excellent organisation. For the first time in our 11 years of missions, we received a complete patient list with age and diagnosis before our arrival, allowing us to review all cases on Sunday afternoon and plan each surgical day efficiently.



Equipment and Supplies
During months of communication via email and WhatsApp, we gathered information about the hospital’s equipment. It became clear that an additional electrosurgical unit was needed. We therefore submitted a funding request to the Fundació Antonius Musa, which kindly provided €1,500 for purchasing the new unit and some surgical instruments (mosquito forceps, clamps, retractors).
The operating area was arranged with three tables, dedicating the one with the functional anaesthesia tower to paediatric and more complex cases. Only one of the hospital’s two electrosurgical units worked, so we alternated the new one we had brought between the other two tables for simpler cases, including bilateral and recurrent hernias.
Only one operating room had overhead lighting, so — as in many African hospitals — we recommend the use of headlamps. Based on our previous experience in Kenya, we advised Dr Garvin to purchase 200 disposable sterile gowns (€400), which were financed by a brotherhood in Seville. We also bought about 25 new diathermy electrodes, financed by a solidarity contribution from Valladolid and Tarragona.
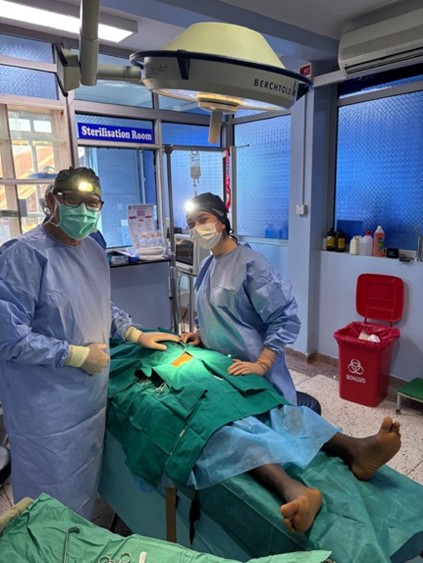

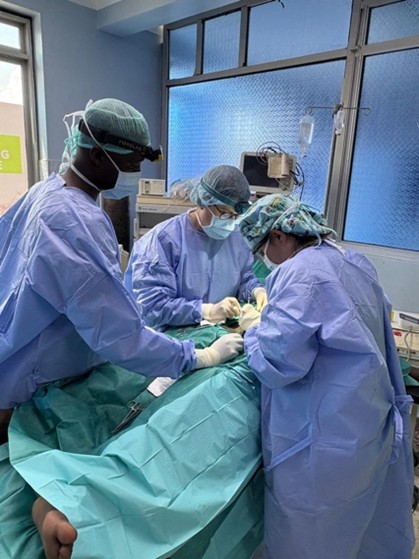
The operating rooms were spacious and air-conditioned, with running water for scrubbing, a toilet, and two changing rooms. Anaesthesia was general for paediatric patients and adults with large midline hernias, while most other patients underwent spinal or local anaesthesia, occasionally with sedation.
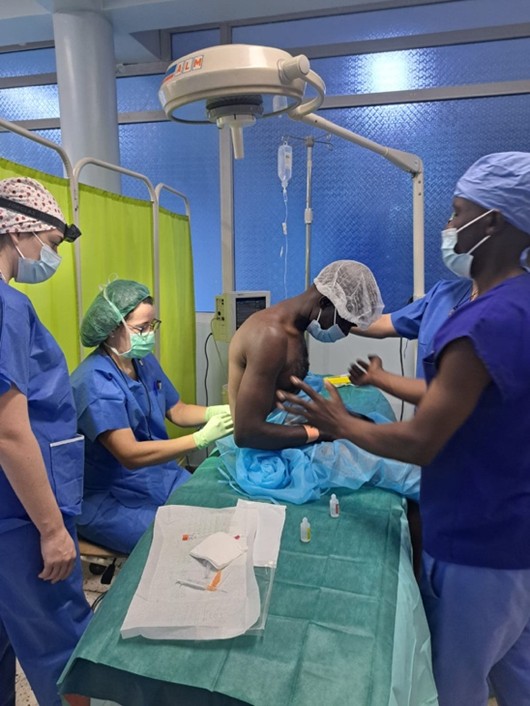
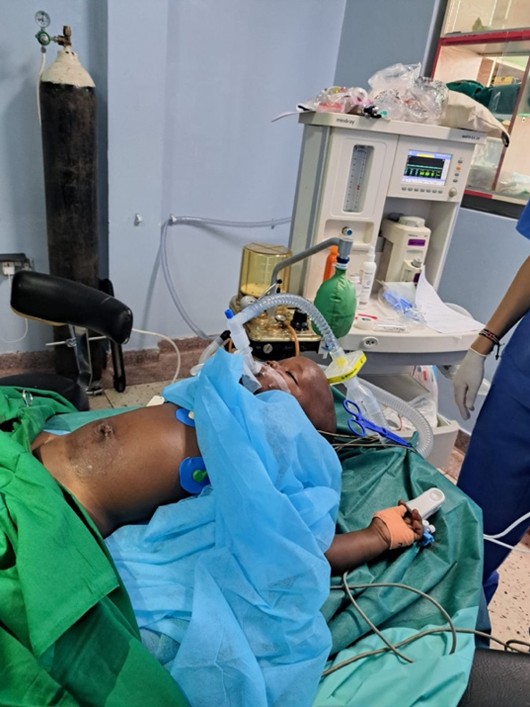
Our contribution also strengthened the hospital’s surgical set with new scissors (Mayo, Metzenbaum), mosquito forceps, Kocher clamps, and other instruments.
Daily Life at Herona Community Hospital
Compared to other Ugandan destinations, Kisoga is less than 100 km from Entebbe Airport. However, due to heavy traffic and densely populated areas such as Kyengera, Nakigalala, Bweyogerere, Namanve, and Mukono, the journey takes over three hours.


The trip was organised through the Tarragona-based agency Viatges Berga, which has arranged our missions for years. Flights were booked with Turkish Airlines, departing from Barcelona — chosen for their cost and convenient arrival time (early Sunday morning), allowing us to travel by daylight and reach Kisoga in time to prepare for the week ahead.
In coordination with Dr Garvin, we obtained import permits for our medical supplies and the electrosurgical unit. The latter’s authorisation was delayed until Sunday morning, causing some hours’ delay at the airport, but thanks to Dr Garvin’s efforts and the local Ministry of Health representative, the issue was resolved. We later had the opportunity to thank them personally during the farewell dinner on Thursday evening.
Due to limited hotel availability, the hospital rented a house for our use, complete with cooks and security guards. Located about ten minutes from the hospital, daily transport was organised for the team (departing 7:30 a.m. and returning at the end of the day — sometimes after 8:30 p.m.).



On Sunday afternoon, after the hospital’s welcoming ceremony with music, we presented the team to the patients and families. Each patient was then examined to confirm diagnoses and plan the surgical schedule for the week.
We began operating on Monday morning at 8:00 a.m., finishing around 7:00 p.m. each day after reviewing all post-operative patients. Most were discharged after 24 hours. On Friday, we travelled to Entebbe for our early Saturday morning flight.

Lunch was served daily around 2:00 p.m. at the hospital, prepared by the same cooks from our accommodation, followed by afternoon sessions.


Patients and Procedures
During the four and a half days of surgery, we treated a total of 88 patients and performed 95 procedures.
- Adult patients: 76 men and 20 women (aged 18–84)
- Paediatric patients: 12 (aged 18 months–17 years)
Conditions treated:
- Inguinal hernias: 68 (7 bilateral)
- Femoral hernias: 5
- Epigastric hernias: 5
- Umbilical hernias: 11
- Hydroceles: 4
- Lymphadenopathy: 1
- Epidermoid cyst: 1
Conclusions
Since its founding in 2013, Herona Community Hospital has continued to grow in infrastructure and equipment, benefiting from the support of various international organisations. Recently, Professor Andrew Kingsnorth visited the hospital, donating an autoclave paid for by Hernia International, for sterilising LDPE (mosquito mesh) hernia prostheses and proposing a training programme for local surgeons in the Lichtenstein hernia repair technique.
During our campaign, our team trained two young surgeons who assisted in most operations, with particular focus on Lichtenstein’s method.
Dr Mukalazi Henry Garvin organised the campaign meticulously, carrying out preliminary patient selection months in advance and overseeing all local arrangements throughout the mission.
For future missions, the hospital would benefit from additional overhead lighting and repairing the broken electrosurgical unit, allowing three fully operational tables. The dedication and collaboration of the local surgical and nursing teams greatly facilitated our work.
Accommodation in the rented house, with cooks and security provided by the local police, proved to be an excellent solution.
Budget Summary
| Item | Cost |
| Flights | €730 + €225 (from Seville) |
| Travel insurance | €65 |
| Accommodation & breakfast | US$200 |
| Meals (lunch & dinner) | US$130 |
| Transport (entire group) | €500 |
| Uganda visa | US$50 |
| Temporary registration (one surgeon) | US$400 |

Report prepared by:
Francesc Marsal Cavallé
Campaign Coordinator