POLICE HOSPITAL FREETOWN MISSION 2026
TECHNICAL REPORT
DATES AND DEPLOYED LOGISTICS
- Mission Dates: January 31 to February 11, 2026.
- Adult Patients: Inguinal, umbilical, and ventral hernias; goiters, lipomas, and sebaceous cysts.
- Total Procedures: 171.
- Total Patients: 158.
- Complications (7 days post-op): 1 scrotal hematoma, 1 acute urinary retention (AUR), and 1 metamizole allergy.
- Complications (1 month post-op): 2 reported complications: 2 seromas

CAMPAIGN REPORT
1. MISSION MEMORANDUM
A. THE SETTING
Sierra Leone faces one of the most complex healthcare scenarios in West Africa, characterized by a high burden of communicable diseases, extremely unfavorable maternal and child health indicators, a fragile healthcare system, and growing challenges derived from non-communicable diseases. Despite recent progress in access to essential services, health outcomes remain suboptimal, and significant territorial and socioeconomic inequalities persist.
Communicable diseases constitute the primary cause of death and illness in the country. Malaria is the single largest healthcare concern, accounting for approximately 38% of all hospital admissions. Tuberculosis remains a major public health issue, with an estimated three new infections per 1,000 inhabitants annually. The national HIV prevalence stands at around 1.5%, remaining relatively low compared to other countries in the region, although significant challenges persist regarding early diagnosis and access to treatment.

The country was severely affected by the most extensive Ebola virus disease epidemic in recent history. Between May 2014 and March 2016, 8,706 infected individuals were recorded, of whom 3,590 died. This episode not only caused high direct mortality but further weakened an already vulnerable healthcare system, affecting public trust, the availability of professionals, and the continuity of essential services. The risk of epidemics and other public health events remains high, given structural limitations in epidemiological surveillance and response capacity.
In the field of maternal and child health, Sierra Leone presents some of the most concerning indicators worldwide. It is estimated that the country has the highest maternal mortality rate globally. Infant mortality is also very high. In 2014, nearly one-third of children under the age of five showed signs of stunting, a reflection of chronic malnutrition. Anemia constitutes a severe public health problem, affecting approximately 70% of pregnant women and 76.3% of children under five. These data evidence significant deficiencies in nutrition, prenatal access, safe obstetric care, and basic pediatric services.
Simultaneously, non-communicable diseases and injuries are emerging as a growing health concern. This phenomenon is linked to the high prevalence of behavioral risk factors such as tobacco use, unhealthy diets, sedentary lifestyles, and harmful alcohol consumption. Pathologies such as cardiovascular diseases, cancer, diabetes, and chronic respiratory diseases, as well as trauma and mental health disorders, increasingly contribute to premature mortality and disability. This situation creates a “double burden of disease,” where communicable and non-communicable pathologies coexist within a healthcare system with limited resources.
While progress has been made in expanding access to essential health services, health outcomes remain insufficient nationwide. Significant inequalities persist in access and health results across different districts and income levels. Geographical, economic, and structural barriers hinder equity in healthcare delivery.
In response to these challenges, the country has developed national strategies and plans aimed at increasing access and improving the quality of essential services, with the objective of saving lives, preventing disease, promoting health, and providing curative care and psychosocial support to those affected. However, consolidating these efforts requires sustained investment, institutional strengthening, the development of healthcare human resources, and improved system governance.
Overall, Sierra Leone faces a complex healthcare landscape defined by high epidemiological vulnerability, structural weakness of the health system, and profound social inequities. International cooperation and local capacity building remain fundamental elements for advancing toward a more resilient, equitable, and sustainable healthcare system.

The Police Hospital, located in Kingtom, Freetown, is a healthcare center belonging to the Sierra Leone Police (SLP) that has historically provided medical care primarily to police members and their families. Its primary function is to ensure the physical and mental well-being of police officers, providing preventive, curative, and emergency services, as well as occupational health support, vaccination, and medical response during security operations. Additionally, the hospital is part of the Police Medical Services Directorate, which collaborates with national and international health institutions to expand its reach and strengthen its care capacities.
In recent years, the Police Hospital has undergone a process of transformation and service expansion, evolving from a limited center for police personnel to a hospital with broader care capacity and community impact. This evolution has been driven by both the SLP leadership and partnerships with international medical organizations. One of the most notable initiatives was the collaboration with the Surgeons in Action Foundation, thanks to the efforts of Dr. John Konteh, which has carried out multiple free surgical campaigns at the center, providing specialized care not only to police officers and their families but also to the vulnerable civilian population. These campaigns have enabled hundreds of surgical procedures—including general surgery—and provided key medical equipment, such as anesthesia machines, tangibly improving the hospital’s technical capacity.
Beyond these campaigns, the center has expanded its infrastructure with the opening of services such as an ophthalmology clinic and the construction of a morgue, as well as the stated intention to develop a nursing school to train local healthcare professionals. These improvements reflect an institutional leadership committed to strengthening the hospital’s resolving capacity and consolidating it as a relevant healthcare resource within Freetown. Another important aspect is the use of the Police Hospital as a space for clinical training and teaching. Under the direction of the Medical Superintendent, the hospital has served as a learning platform for local healthcare professionals, contributing to reducing dependence on foreign personnel and gradually raising the medical competencies available in Sierra Leone. Although the Police Hospital is not a direct part of the network of public hospitals managed by the Ministry of Health and Sanitation (such as Connaught Hospital or Princess Christian Maternity Hospital), its role has expanded through public-private partnerships and international cooperation, especially in contexts where the need for specialized services exceeds the capacity of traditional public hospitals.
Our activity was developed exclusively in the surgical block, located in a two-story building separate from the rest of the complex. This building features 3 consultation areas (one of them being Dr. Konteh’s office) and 3 hospitalization wards; we used the two larger wards for men and the smaller one for women, typically for thyroid pathologies. The total capacity is 28 beds, which were used entirely for the campaign, occupying the whole floor for our work. At the end of the hallway is the access to the operating room area, which maintains a sterile circuit with two large ORs connected by a shared sterile room and hand-washing station. Likewise, in the hallway, there is a room with a long table used for our meals and coffee, in direct contact with OR 1.
There is a new anesthesia machine, a Dräger Atlan A300 model, featuring mechanical ventilation (VC and PC), a sevoflurane vaporizer, and perfectly functioning capnography. The operating rooms are equipped with split air conditioning units, allowing for comfortable work over many hours despite high outdoor temperatures. However, power outages occur frequently, requiring the units to be restarted and causing moments of sweltering heat. The sterile area is where local staff work diligently to sterilize gowns, drapes, and instrument sets. On the upper floor, there is a nursing duty room used as a storage area for surplus material from previous campaigns and as a changing room for the volunteers.
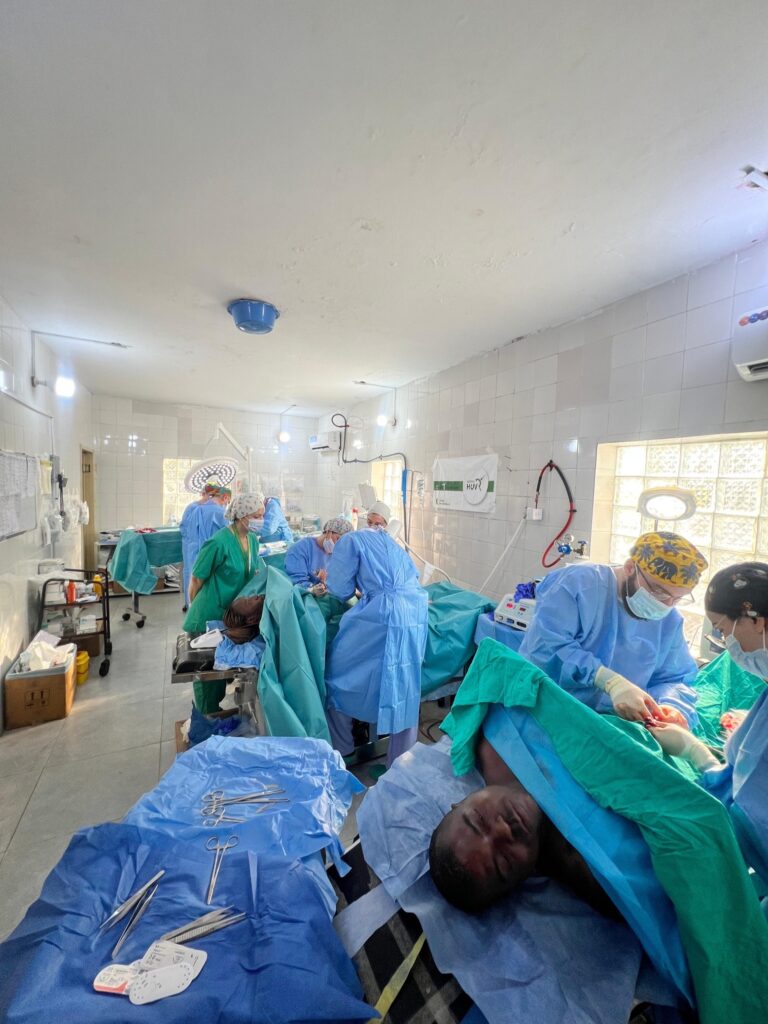
As per our campaign custom, and despite initial reluctance from local staff, we structured OR 1 (the larger of the two on the left) to accommodate 3 surgical tables. This setup, while not excessively spacious, was functional and allowed enough room for patients to enter on stretchers (Photo 1) so we could work together. Based on the experience gained from our previous 8 campaigns, staying together, working together, and taking breaks for meals and coffee as a group is fundamental to the work environment and team relationship. OR 2 was utilized as a Kanban area.
B. THE TEAM (Group Members)
The team specifically comprised General Surgery specialists Eduardo Perea, Manuel Bustos Jiménez, Abdul Razzak Muchref Al Dandal, Carlos Javier García Sánchez, Jose María Álamo Martinez, and Ángela de Jesús Gil; Surgical Resident Beatriz de los Ángeles Ruiz García; Anesthesiologists Alejandra Abasolo Ibañez, Ordoño Rodrigo Alonso Tuñon, and María del Mar Martínez Gómez; and Daniel Luis Nadales Muñoz as the Nursing lead. This year, an additional surgeon joined the team to manage outpatient consultations and morning ward rounds without delaying operating room (OR) activity, as well as to relieve the more experienced surgeons during afternoon shifts without affecting the surgical schedule.

Despite initial reservations regarding such a large group, it was proven that in a facility with such extensive local support and availability, a large team capable of operating on three tables simultaneously—while simultaneously triaging patients, managing discharges, and addressing unforeseen events such as emergencies or gastrointestinal illnesses among team members—resulted in a success in both the volume and the quality of care provided.
C. LOCAL STAFF
The hospital provided a large and available local team; the experience was overwhelmingly positive in terms of the involvement of both OR and ward staff, exceeding that of previous campaigns. Participants included:
- Dr. John Konteh: His role was exceptional, managing massive patient recruitment with precise pathologies, providing follow-up for post-operative patients, resolving emergencies, and assisting the volunteer physicians with basic needs, accommodation, transport, and currency exchange. His 24/7 availability and the provision of missing materials ensured a continuous sense of institutional backing from the Police and the center.
- Security Personnel: They provided transport from the hotel and accompanied the team during consultations and within the hospital. Special mention goes to Abu Marah, who was always helpful and managed traffic control.
- Police Nurse Liaison: Mohamed served as the campaign coordinator and our primary point of contact, maintaining direct communication with Dr. Konteh. Although initially shy, his efforts were essential for the seamless operation of the mission.
- Outpatient Assistant: Marie provided an admirable spirit and joy to the center. She prepared the consultation rooms, ensured a constant supply of fresh water, and managed the arrival of new patients for screening.
- Ward Staff: 4 to 6 nursing assistants/nurses monitored patients postoperatively and managed intravenous access. Nurses Davide and Vintu were particularly notable for their dedication to patient mobilization, monitoring vital signs, and pain control, as well as assisting in consultations.
- Operating Room Staff: 2 to 7 members performed various roles, from cleaning to porterage, ensuring the agile transfer of patients. Two nurses possessed basic anesthesia knowledge (Yabah and Francis), and two others served as circulating or scrub nurses. Their constant presence throughout the day was a vital asset.
- Sterilization Lead: Kabba was responsible for the sterile supply, constantly providing gowns, drapes, and instruments for three surgical tables, even as our own supplies began to dwindle.

D. EQUIPMENT
The OR consists of three surgical tables. There is one electrosurgical unit (ESU) that only supports a single terminal. Various sutures remained from previous campaigns. No surgical meshes are available locally. Two monitors with pulse oximetry and BP cuffs are provided.
E. ANESTHESIA
The OR is equipped with a Dräger Atlan A300 ventilator capable of VC and PC mechanical ventilation, a Sevoflurane vaporizer, and perfectly functioning capnography. Oxygen cylinders (up to 4 or 5 available), saline solution, and IV catheters are on-site. The supply cabinet contains some ampoules of norepinephrine, bupivacaine with dextrose, and epinephrine. Two monitors are available, though their operation is inconsistent.
F. ASEPSIS AND SURGICAL MATERIAL
Basic surgical sets contain sufficient but deteriorated instruments. Organization was challenging as we had to include all the instrument sets we intended to use. However, sterilization was completed within an hour, allowing for rapid turnover. Cloth gowns and drapes are similarly autoclaved. Given the high volume of interventions, it is recommended to bring additional gowns and drapes, as sterilization times sometimes lagged behind demand. Bringing a portable ESU is advisable; in this mission, we brought an ESU and a Ligasure device to enable simultaneous surgery on three tables.
G. ACCESSIBILITY FOR THE POPULATION
The hospital is highly affordable and accessible; patients were not charged for surgery or admission. Imaging and laboratory tests are available at a separate facility for a reasonable fee. The team noted that the treated population was in significant need and lacked easy access to alternative healthcare. All medication was provided by our team, with surplus stock donated to Dr. Konteh.
H. LIFE IN FREETOWN
The preparation and success of the campaign at Police Hospital were inextricably linked to the collaboration of Dr. Konteh and Mohamed. They actively participated in logistics, including airport pickup and negotiating rates at local hotels. We noted that the country and the campaign in general were more expensive than in previous years. The Jam Hotel was selected for its proximity and price.
- Day 1: Departure from Seville to Malaga by bus, followed by a flight. Arrival in Freetown at dawn after a 5-hour layover in Casablanca. Dr. Konteh facilitated customs and security, avoiding fees. After taking the ferry to the capital, the team went directly to the hospital at 8:30 AM to set up the OR and screen patients. Over 200 patients were waiting. While Anesthesia and Nursing organized 22 suitcases of equipment, the surgeons divided into teams to perform screenings and complete surgical schedules. The day ended at 6:00 PM.
- Day 2: Reception at the Police Headquarters followed by a 10-minute drive to the hospital. Due to roadworks and chaotic traffic, walking is discouraged. Consultations and surgeries began on three tables. The first day concluded with 24 patients treated.
- Days 3–10: Incessant OR activity due to a “call effect” that drew a high volume of patients. Over 250 patients were seen in consultation. Local staff showed impeccable commitment. On Saturday the 7th, the team visited the MercyShip Africa, establishing a cordial relationship to ensure follow-up for patients remaining on the waiting list.
- Day 10: On the way to the center, the team assisted a 14-year-old girl struck by a motorcycle. The final 12 scheduled cases were completed in the morning. At the last moment, a painful incarcerated umbilical hernia arrived as an emergency and was treated. Following a brief visit to a local market and a farewell dinner with the hospital staff, the team departed for the airport at night.
I. IMPLEMENTATION OF IMPROVEMENTS
As in the previous year, we have included this section, which we consider essential as it is the result of 9 campaigns conducted by this family of volunteers alongside Surgeons in Action.
The role of our local counterpart, Dr. Konteh, has been absolutely vital for the development of the campaign and the achievement of results. His involvement allowed for pre-arrival coordination and the transportation of patients from remote locations (up to 300 km away) for surgery. Similarly, we have secured the assistance of Mohamed, who will manage a local terminal to provide support and follow-up for patients who underwent thyroidectomies.
Based on our satisfaction surveys from the previous year, we have improved patient care, the protection and defense of privacy, and communication and information delivery during consultations. We also identified affordable pharmacies where patients can obtain Thyroxine. Simultaneously, two scientific projects were conducted by medical students from the University of Seville, focusing on the role and impact of cooperation campaigns on local healthcare activity.
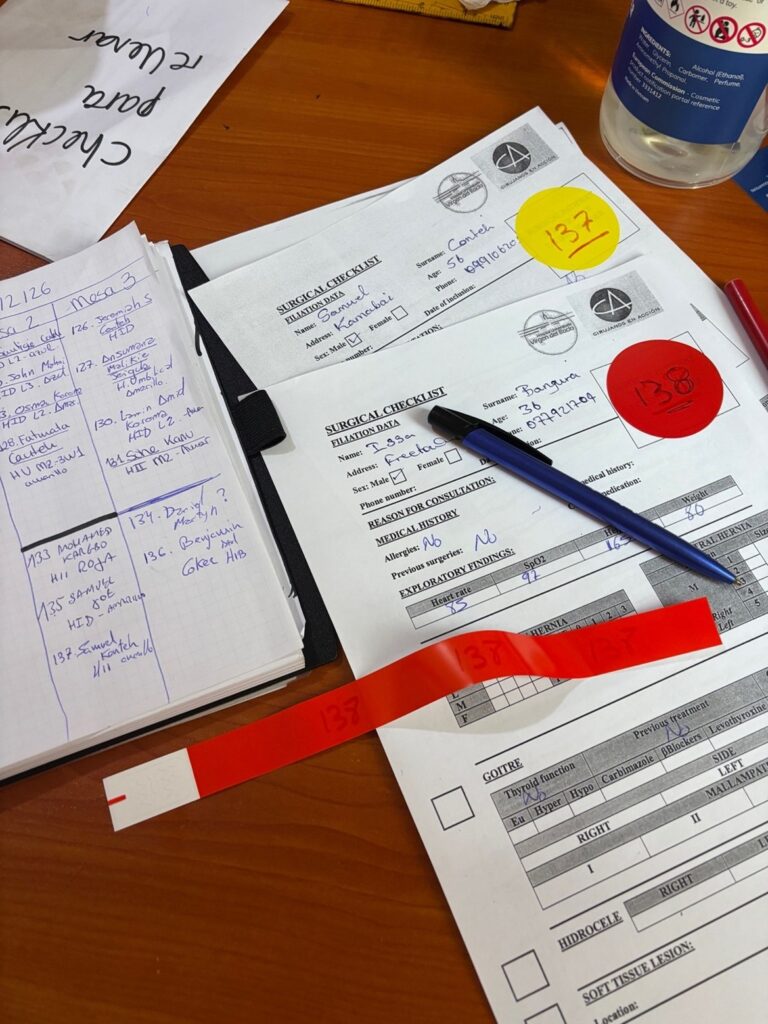
We continue to refine our patient CHECKLIST system, which we will share with other Surgeons in Action missions. This tool facilitates patient screening and ensures compliance with quality standards.
A color-coded identification system using wristbands and stickers has been implemented. This system highlights potential surgical or anesthetic difficulties and provides visual alerts for HIV-positive patients or those with specific allergies.
J. PATIENT FOLLOW-UP
The Surgeons in Action 2026 project is designed, as it was in previous years, to ensure the follow-up of all surgical patients. Thanks to the collaboration of Dr. Konteh and Mohamed, a monitoring plan has been established, including follow-up calls for thyroid patients to monitor clinical symptoms and treatment adherence.
Additionally, a WhatsApp group has been created for hernia patients to address concerns and ensure proper follow-up. Wound reviews will be conducted at the local hospital by trained nursing staff, and thyroid treatment follow-up will be managed by the hospital’s Endocrinologist for the patients operated on during this mission.
K. RESULTS
| Variable | Resultado (N = 158) |
| Sexo masculino | 127 (80.65%) |
| Edad (Media [SD]) | 44.22 [±19.16] años |
| Color (Triage) | Verde: 5 (3.2%) Amarillo: 48 (31.0%) Azul: 84 (52.3%) Rojo: 21 (13.5%) |
| Alergias | 2 (1.29%) |
| HTA | 20 (12.90%) |
| Diabetes (DM) | 5 (3.23%) |
| Medicación domiciliaria | 25 (16.13%) |
| Diagnóstico | N (%) |
| Hernia inguinal | 98 (63.23%) |
| Hernia inguinal bilateral | 13 (8.39%) |
| Hernia ventral | 10 (6.45%) |
| Lipomas y tumores blandos | 1 (0.65%) |
| Bocio | 21 (13.55%) |
| Hidrocele | 5 (3.23%) |
| Criptorquidia | 1 (0.65%) |
| Hemorroide | 1 (0.65%) |
| Frenillo | 1 (0.65%) |
| Quiste sebáceo | 1 (0.65%) |
| Onfalocele | 1 (0.65%) |
| Procedimiento | N |
| Liechtenstein | 103 |
| Nyhus | 0 |
| Rives | 5 |
| Hemitiroidectomía | 10 |
| Tiroidectomía subtotal | 3 |
| Tiroidectomía total | 7 |
| Hidrocele (cirugía) | 5 |
| Orquiectomía | 1 |
| Exéresis | 4 |
| Herniplastia preperitoneal | 1 |
| Drenaje de absceso | 0 |
| Herniorrafia | 5 |
| Hemorroidectomía | 1 |
| Istmectomía tiroidea | 1 |
| Variable | N (%) |
| Incidencias intraoperatorias | 3 (1.94%) |
| Reintervenciones | 0 (0%) |
| Náuseas | 4 (2.58%) |
| Retención urinaria | 2 (1.29%) |
| Sangrado herida | 0 (0%) |
| Hematoma | 1 (0.65%) |
| Seroma | 0 (0%) |
| Parálisis recurrencial (disfonía) | 1 (4.76%)* |
| Tiempo | N (%) |
| Ambulatoria (0 días) | 131 (84.52%) |
| 1 día | 23 (14.84%) |
| 2 días | 1 (0.65%) |
| 3 días | 0 (0%) |
L. SCIENTIFIC ACTIVITY
Data has been collected for two Undergraduate Dissertations (Final Degree Projects) by two final-year medical students from the University of Seville. The purpose of these studies is to analyze the impact of cooperation campaigns on the host centers and populations, evaluating the evolution of healthcare delivery models and the potential application of Artificial Intelligence (AI) in surgical cooperation missions.
The analyzed data and resulting conclusions will be shared with both Surgeons in Action and the leadership of the host center.

2. CONCLUSION
Strengths of this location:
- Strategic Location: High density of population in need with limited access to surgical personnel.
- Exceptional Local Collaboration: The local hospital staff is accustomed to several campaigns per year, making them highly familiar with this type of medical activity.
- Institutional Network: A significant number of Spanish foundations and NGOs operate in Freetown, which aids in reaching vulnerable populations. This allows for high patient recruitment and a reliable local counterpart that facilitates patient preparation and follow-up.
Objectives for Improvement:
- High Campaign Costs: Expenses related to transportation, lodging, and meals remain high.
- Endocrine Surgery Specialization: It is recommended to include an endocrine surgeon. Although hernias are the primary objective, the area is endemic for goiters and Graves’ disease. While the local staff maintains the hernia OR, they are particularly interested in resolving thyroid issues, which are rarely addressed in the capital.
- Energy Sources: Ensure the availability of additional energy sources (electrosurgical unit or Ligasure for goiters).
- Team Capacity: The hospital accommodates large, multidisciplinary teams effectively.

3. BUDGET (Breakdown of Expenses)
COST PER PARTICIPANT:
- Round-trip flights (including medical equipment check-in): €1,100
- Bus transport: €50
- Ferry: €100
- Accommodation (Hotels): €400
- Meals: €200
- Local transport and others: €0 (Funded by Police Hospital)
Total cost per participant: €1,850
TOTAL CAMPAIGN COST: Approximately €20,350
Fdo: Eduardo Perea del Pozo Responsable de la campaña Police Hospital 2026
Cirujanos en Acción