FARAFENNI CAMPAIGN (GAMBIA). OCTOBER 20-29, 2023
STATUS: COMPLETED
Coordinators: Inma Giménez, Jose Mª Guallar
General Surgeons: José Mª Guallar, Berta Lluch, María Dolores Periañez, Ainhoa Andrés, Enrique Colás
Paediatric Surgeon: Rocío Lizarraga
Anesthetists: Francisco Llácer, Inma Giménez
Nursing Team: Javier Madrazo, Esperanza Galarza, Míriam Martínez
Total: 11 volunteers

REPORT
Given that Dr. Eduardo Perea’s report from last year was very helpful, I am borrowing his structure and incorporating common aspects for future missions.
TECHNICAL REPORT:
DATES AND LOGISTICS DEPLOYED:
Campaign conducted from October 20 to October 29, 2023
ADULT PATIENTS: Hernias (inguinal, umbilical, ventral, and inguinoscrotal), hydroceles, supernumerary breasts, ganglions, condylomas, lipomas, and sebaceous cysts.
PAEDIATRIC PATIENTS: Hydroceles, umbilical hernias, keloids ear/circumcisions, prepucial cysts, inguinal hernia, retractile scars, colostomy prolapse.
CONSULTATION AND SURGERY PERFORMED
Total procedures: 101 procedures
Total operated patients: 96 patients (including 33 paediatric patients, aged from 9 months to 11 years)
Patients seen in consultation: 161
Complications (within 7 days of our arrival):
– 2 seromas in inguinoscrotal hernias
– 1 seroma in supernumerary breast
– 1 folliculitis
– 2 cellulitis in pediatric umbilical/inguinal hernias
CAMPAIGN SUMMARY
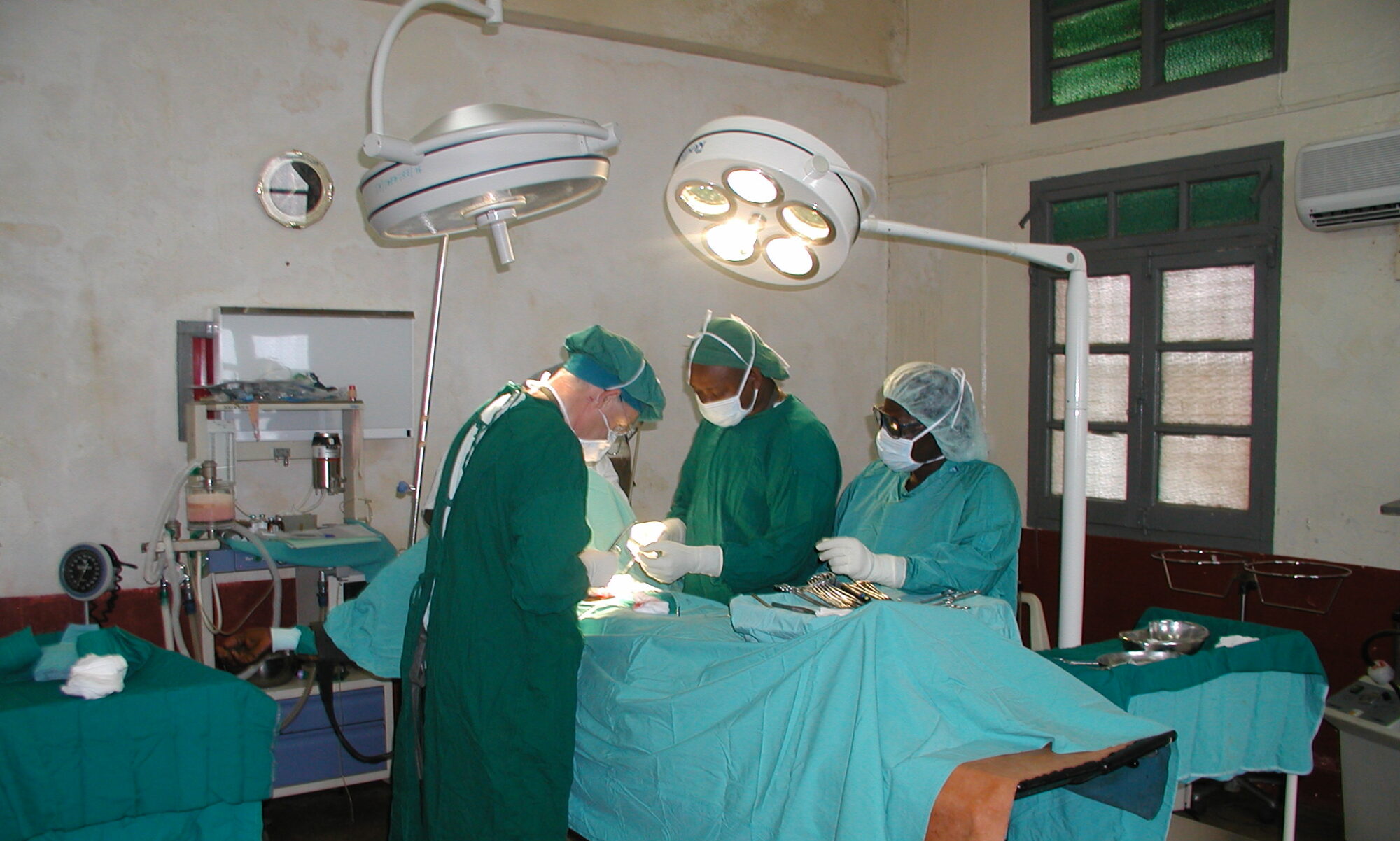
THE LOCATION
Farafenni General Hospital was established in 1999 as part of the Gambian government’s effort to create a healthcare center of reference in the eastern part of the country. It is a well-equipped and organized large center with 250 beds, of which 175 are currently occupied, due to human resource limitations.
Farafenni is a small inland town strategically located next to the only bridge across the Gambia River, making it a transit point for local trade and travel between different parts of Senegal.
The population is approximately 25,000, providing services to both Gambian and Senegalese residents. While English is the official language, Wolof and Mandinka are the commonly spoken languages among the population.
The hospital is divided into an initial area for administrative offices and emergency care, and a nearby building for laboratory and testing, which connects to different wings for surgical patients, maternity, pediatrics, internal medicine, and dentistry, each with two floors.

In the surgical wing, there is a clean circuit with two large operating rooms, one dedicated to maternity and the other for general surgery. Each operating room is equipped with a basic ventilator capable of using halothane and an diathermy generator.
The operating rooms are equipped with split air conditioning, allowing comfortable work despite the high outdoor temperatures.
Obstetric material is not used due to the high number of emergency cesarean sections.
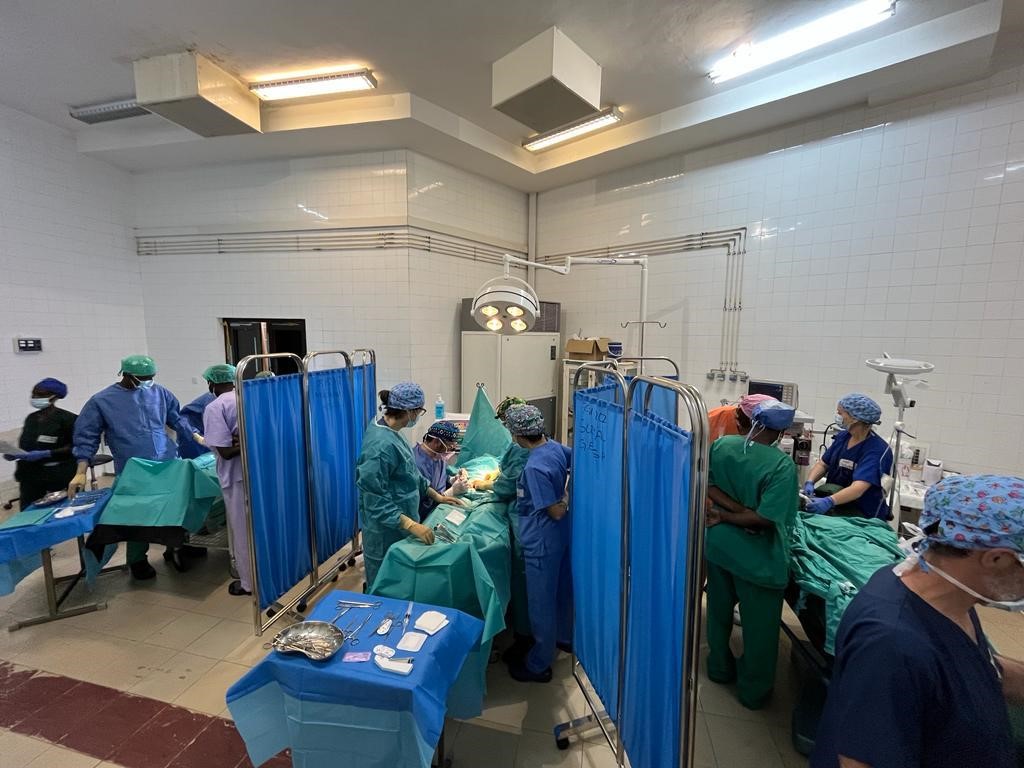
The surgery room can be configured to accommodate three tables simultaneously while allowing for easy patient entry and exit on stretchers.
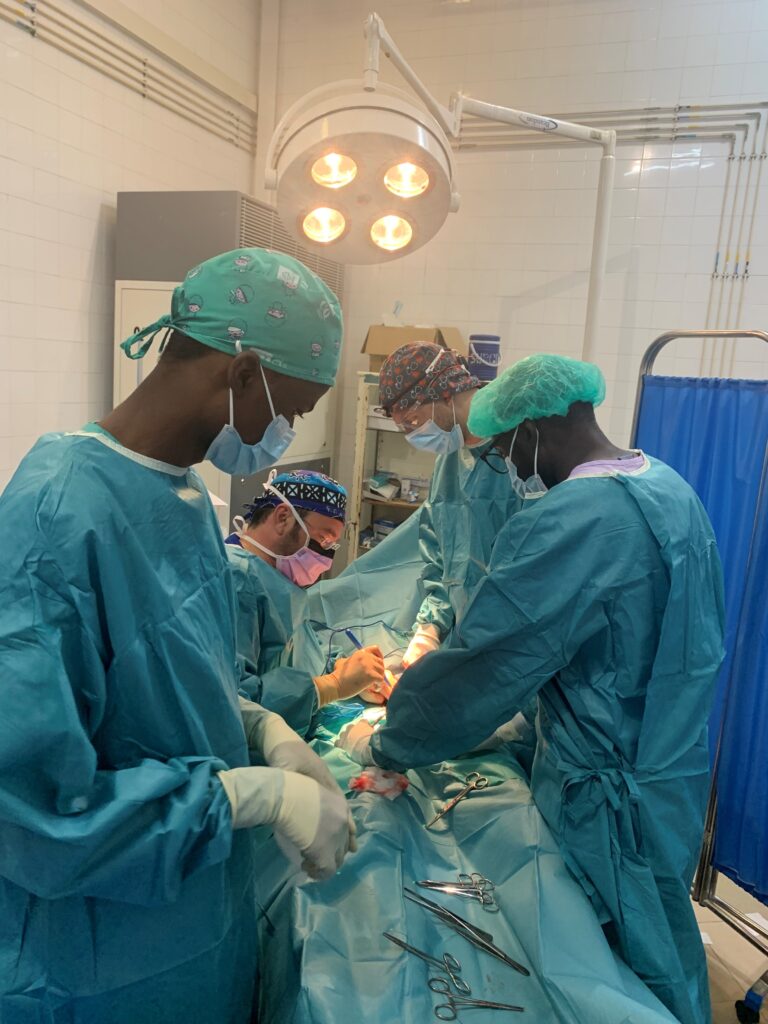
THE TEAM
This time, we had a larger team than usual, consisting of five general surgeons, one pediatric surgeon, two anesthesiologists, and three nurses (you can find their names at the beginning. ( See Photo 2).
LOCAL STAFF
The hospital has a competent local staff that has been of great assistance. Thanks to our contact with a Cuban surgeon based there (Dr. Alain), we were able to operate on 16 patients on the first day (this would not have been possible without his prior patient selection).
Local nursing and auxiliary staff, including instrument specialists, anesthesia nurses, circulating nurses, orderlies, and cleaning staff, proved to be highly competent (see Photo 3).
The hospital also has a reception/recovery room where peripheral venous access is established before entering the operating room, facilitating the start of surgeries, especially for younger children.
EQUIPMENT
Given our larger team and the fact that it had been done in previous campaigns, we requested to work with three operating tables.
The hospital has one diathermy generator that can accommodate only one terminal. We brought various sutures from previous campaigns, but there were no meshes available.
There was only one monitor with a pulse oximeter and a blood pressure cuff, without an ECG.
ANESTHESIA
The operating room is equipped with a ventilator and two vaporizers for halothane and isoflurane, but only the first gas was available.
We primarily used the table where the ventilator was located for paediatric surgeries.
We could work with manual and controlled IPPV ventilation, although monitoring the method of ventilation was not easy, we could assess tidal volume and respiratory rate, but there was no capnography.
Additionally, there was an oxygen condenser that could be used with a Mapelson if two general anesthesias coincided.
They had normal saline, abocaths, spinal anesthesia needles, and bupivacaine with dextrose available.
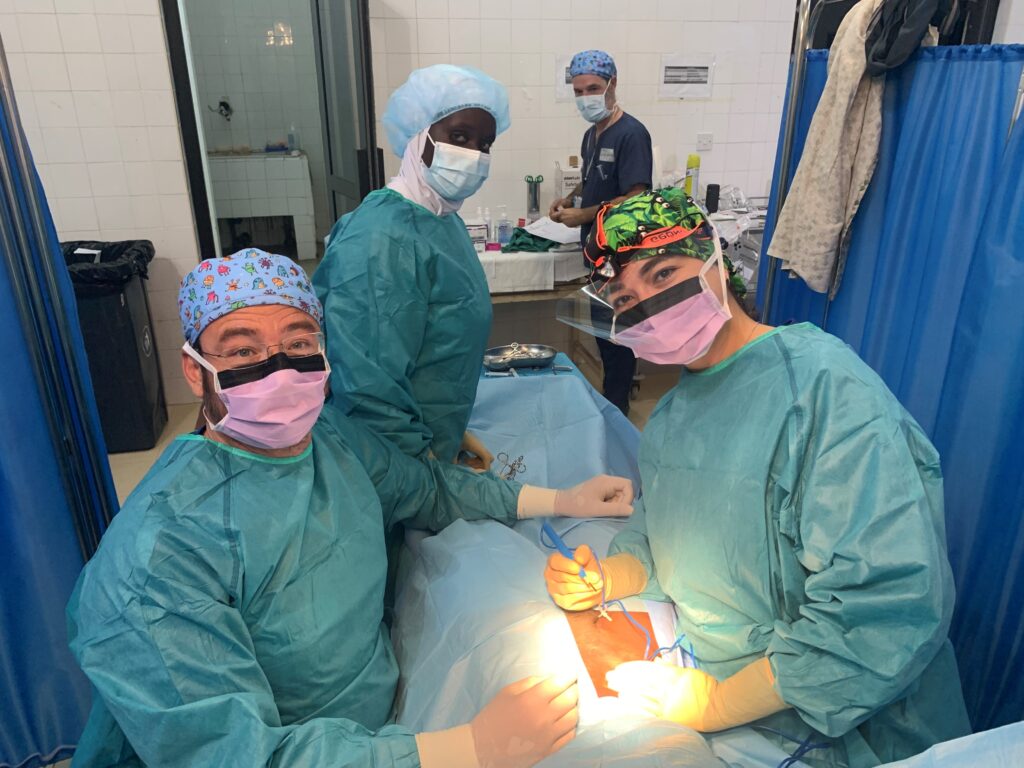
ASEPSIS AND SURGICAL MATERIAL
Basic surgical material boxes were available, with sufficient but deteriorated instruments. There was a laparotomy kit with more equipment than was used during the campaign. Surgical gowns and cloth drapes were sterilized using an autoclave.
Because we had a large team and considering the advice from the previous team, we decided to bring two additional diathermy generators, which allowed us to work on three operating tables simultaneously, even for procedures requiring electrical devices.
Bringing complete surgical drapes, gowns, and other disposable surgical materials and medications was very useful.
ACCESSIBILITY FOR THE POPULATION
The hospital is affordable and accessible to the population, with a charge of 40 Euro cents for Gambian residents and 80 Euro cents for Senegalese residents upon admission. Imaging and laboratory tests are charged separately, but the fees are not excessively high, although some patients may have difficulty paying.
OUR LIFE IN FARAFENNI
We traveled via Barcelona-Casablanca-Banjul, arriving in the capital at 1:30 AM. Mr. Sainey Dibba, the hospital’s logistics officer who helped with hotels, meals, and transportation, was waiting for us at the airport, along with other hospital staff.
This made it much easier for us to clear customs and exit.
From there, we went to a nearby hotel (Lebato Hotel) to rest for a few hours before heading to Farafenni. The rooms had fans and allowed us to take a shower. They also had a beachfront view.
The following morning, we left for Farafenni with two cars. The journey took 3-4 hours on well-paved roads, but it was time-consuming due to traffic.
In Farafenni, we stayed at the Wallyman Hotel, which was a 10-minute walk from the hospital and had a pleasant garden leading to individual air-conditioned rooms (the cost was approximately 110 euros per person for the entire stay).
It’s worth noting the sounds of the nearby mosque with repeated prayers at 5 in the morning :).
Upon arrival on Saturday afternoon, we began unpacking our luggage, which included 22 bags of material and medication. Dr. Alain had already prepared a list of patients for us to assess, but it was mostly on Sunday that they arrived, allowing us to start surgeries on the same day at 9 AM.
Our routine in Farafenni included walking to the hospital in the mornings at 7:45 AM for breakfast before starting surgeries.
Once at the hospital, the surgeons made rounds with patients who had been operated on the previous day, while the anesthesia and nursing teams prepared the surgical tables.
Surgeries would begin, and they continued until 2 PM, when we stopped for lunch at the hospital.
Afterward, we resumed surgeries from 3 PM until 6-7 PM (although some days we finished later, it was not the norm). It was several days of very satisfying work alongside the competent local staff.
On the last day, we met with Dr. Kebba Manneh and the rest of the hospital staff for a debriefing session, where we expressed our mutual gratitude for the successful campaign.
We believe it was successful based on the number of patients operated on and the opportunity to operate on pediatric patients.
Our flight departed in the early hours of Sunday at 2:30 AM, so we traveled in two cars to Banjul after the hospital meeting, accompanied by Mr. Sainey.
We decided to rest for a few hours in a beachfront hotel with a pool. From there, at 10 PM, we headed to Banjul Airport, en route to Casablanca.

CONCLUSION
Strengths of this location:
– Strategic location with a significant population in need
– Presence of a Cuban community with which communication and patient follow-up is easy
– Strong collaboration from the local hospital and its staff in assisting us with transportation, accommodations, and other logistics
– A significant number of Spanish foundations and NGOs working in Banjul and other rural areas can help access the needy population (it would be important to contact them well in advance of the campaign)
Areas for Improvement:
– Difficulty in filling out and sending forms, data, photographs, and other documents in the months leading up to the campaign.
– Creating an inventory of all materials and medications with expiration dates, manufacturers, and quantities is a challenging task when you are carrying 400 kg of luggage like us.
– It is impractical to pay 400 euros for medical registration to work in the campaign (initially requested, but we were later granted scholarships, and it cost us only 30 euros with expenses).
– If possible, bring both an endocrine surgeon and a pediatric surgeon.
– Bring an additional source of energy (electrocautery or Ligasure for thyroidectomies). Note that there is only one available, and we can work on three surgical tables simultaneously.
– The hospital accommodates a large multidisciplinary team.
– Improve patient recruitment so that surgical schedules can be created in advance (in the final days of our campaign, we ran out of patients. We were informed that the best period to go is in the last two weeks of November or the first week of December due to the employment situation of the population).
BUDGET:
COST PER PARTICIPANT:
– Round-trip flights with checked luggage: 480€
– Hotels: 120€
– Food: 100€
– Approx. Transportation and airport fees: 190€
– Miscellaneous: 150€
– Total: 1040€ per participant
TOTAL CAMPAIGN COST: Approximately 11,440€
Yours sincerely,
Inma Giménez Jiménez
Head of the Farafenni Campaign October 2023
Surgeons in Action