The first joint mission of the Surgeons in Action and Hernia International Foundations following the Covid-19 pandemic has been carried out in Bopolu City, a small Liberian inland town of 3200 inhabitants located in Gbarpolu County, home to approximately 90,000 people. It is the first campaign to be conducted in this destination, and the reason is that this is where Dr. Peter George is now working.
Peter George has been the collaborating doctor of our two foundations for many years and is now the head and medical director of Jallahlone Hospital, the reference health centre for the whole county. This is my third campaign in Liberia that I have coordinated with him, and he has always shown great organisational skills and leadership in his country.
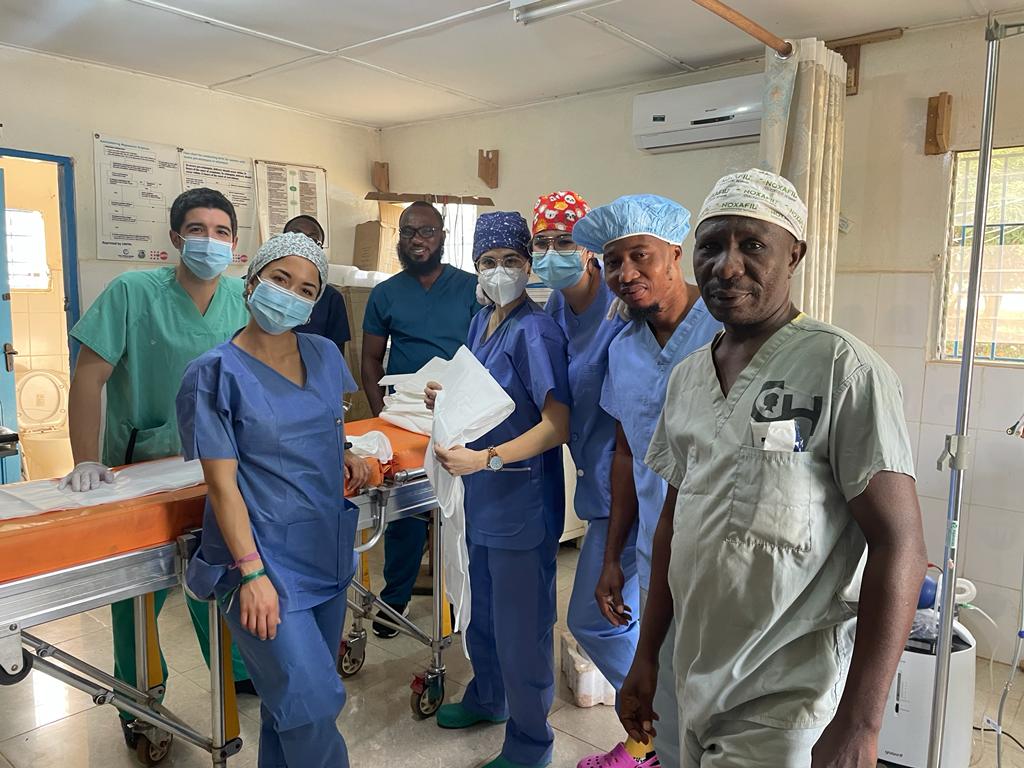
The preparation of the campaign has been very complicated since it was suspended on two occasions as a result of the spread of the Covid pandemic and the restrictions on entry to Liberia even for people from countries with a high vaccination rate and the possibility of carrying out routine diagnostic tests for active infection such as PCR or antigenic tests. On two previous occasions in 2020 and 2021, the campaign was postponed when everything was organised and the plane tickets had been bought, which is why it has meant a great financial, moral and resilience effort on the part of the team members.The team members were three surgeons (César Ramírez, Pablo Muriel and Sarai Ayllón), two anaesthetists (Sandra Casares and Beatriz Fort) and three nurses (Francisco Gómez, Rebeca Sanabria and Julia Cáceres), and we all received authorisation from Dr. Peter George from the Medical and Dental Council of Liberia to practice since our professional documentation was sent electronically. The initial expedition included a fourth surgeon, Marta Roldón from Málaga, who was unable to travel due to a positive PCR test the day before departure.
The departure of all the team members was on Thursday 20th January in the afternoon and we met in the evening in Madrid; Pablo and Beatriz left from Barcelona, Sandra was in Madrid and the rest of the team members from Malaga. The trip was made with Air France (Air Marocq has stopped operating flights to Liberia in the pandemic) and started in the early hours of Friday 21st with the Madrid – Paris flight at 6 a.m. and from Paris we left on Friday 21st at 12.25 p.m. to arrive in Monrovia at Roberts International Airport at 8.25 p.m. on a direct flight. As part of the security protocols we followed in order to get to Liberia, all team members travelled with a certificate of having received three doses of messenger RNA vaccine and a certificate of a negative PCR test carried out at least 48 hours before departure to Paris. Each team member was required to pay $150 for diagnostic tests for active infection on arrival in Monrovia and on departure, and these tests were carried out by airport health staff on arrival and by the laboratory manager at Jallahlone Hospital in Bopolu three days before our departure from Liberia, both of which were rapid antigen tests.Once we had passed the Covid health checkpoint at the airport, Dr. Peter George was waiting for us at the baggage claim (as he always does) to facilitate the logistics of transporting the 23 pieces (over 500 kg) of equipment we had brought, for which we had to pay an excess of 1200 Euros at the airport in Madrid. Since it was after 10 p.m. on the 21st upon our arrival, that night we slept at The Blue Lagoon in Monrovia, an acceptable hotel with a swimming pool available and which is a frequent place for the Liberian middle class. On the morning of the 22nd we left Monrovia for Bopolu, a drive of almost 5 hours to complete a little over 90 km on a road that is terribly bad, full of potholes, rocks and that becomes unbearable at times. We arrived in Bopolu City at 3 o’clock in the afternoon and were welcomed with a big party by the women’s association of the city. There is an important feeling of protection of the role of women and they are looking for a situation of equality that does not yet exist in Liberia, a country where the structure is still very patriarchal. After a warm presentation at the hospital by the health and administrative authorities, we unpacked all the material and placed it in the hospital facilities and then went to our place of residence to take possession of the rooms and carry our suitcases.
Jallahlone Hospital is a medical-surgical centre with the typical structure of small Liberian hospitals located outside the capital, in the style of the one we knew in Ganta City (E&J Medical Center).
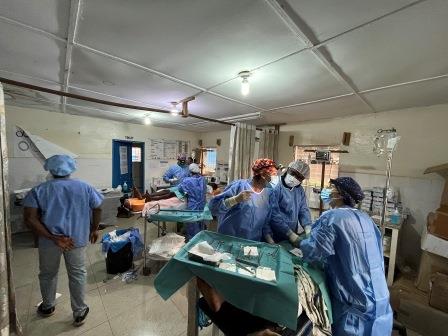
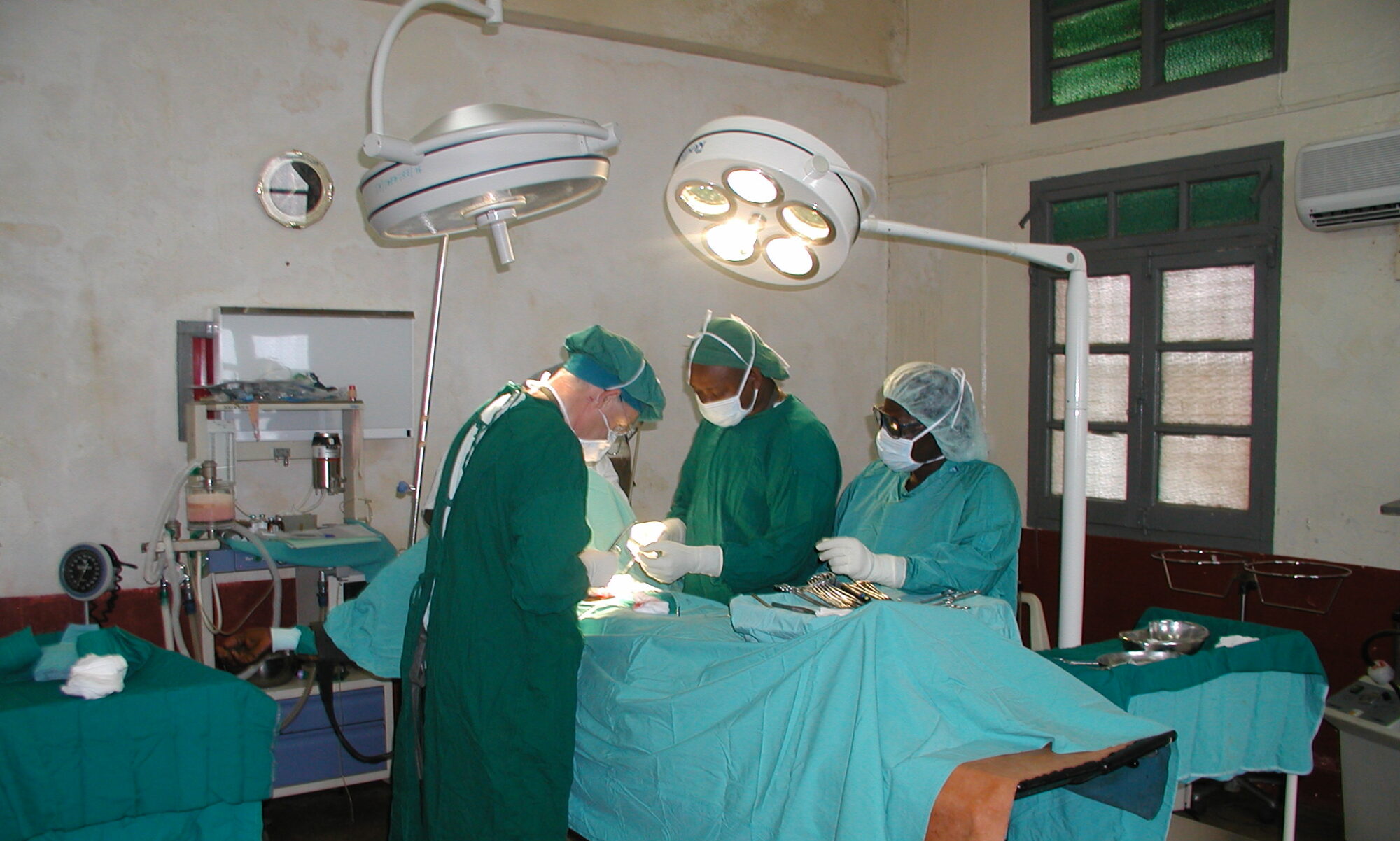
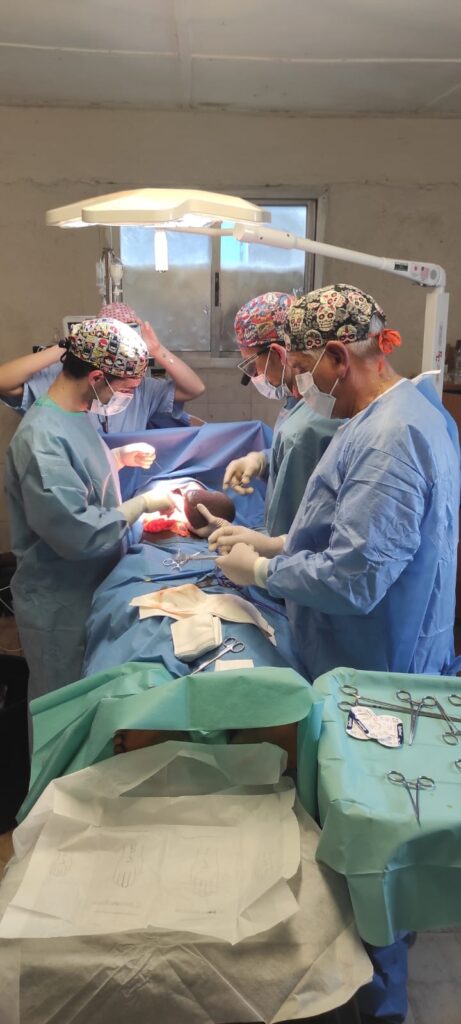
It has an operating theatre equipped with a ventilator in which interventions can be performed under general anaesthesia; the usual activity of this operating theatre outside the campaigns are caesarean sections but also herniorrhaphy (I don’t know how often), hence the large number of reproduced inguinal hernias that have been operated on in this campaign, easily identifiable by the type of incision and because they did not have mesh in place.

There is a hospital ward for men, another for women, another for children and a fourth, a maternity area. The second physical space that we have set up as an operating theatre has been a regular medical care room in which we have placed two stretchers for transferring patients who are somewhat unstable, but which have been used to operate on hernias and major outpatient surgery. In the operating theatres there is only one electric scalpel which works irregularly; we have brought two from Spain and we have given one as a gift to stay there in the Hospital. In the main operating theatre there is no air-conditioning but there is a ceiling light that works acceptably from 10 a.m. onwards, which often goes out and is interrupted; in the other room there is air-conditioning, which makes it more bearable, but there is no light and it is essential for the surgeon and assistant to use headlamps.
There is no wifi network in the hospital or in the whole region, and in order to connect to it we had to buy a router at the airport, which had to be progressively recharged during our stay.The accommodation site was about 300 metres from the hospital and is a building that is not used regularly (there are no visitors or tourists there) and has about 25-30 rooms equipped with a bed (with mosquito netting but with a base of boards that acts as a bed base and usually breaks), a bedside table, a fan and a bathroom that has no electricity or running water (there is a large bucket of about 100 litres from which water is drawn with a ladle to take a shower and clean the toilet for daily needs). The stench is unbearable in the bathroom as the drains run under the shower tray. The food as always in
Liberia is quite acceptable, and Peter makes sure that we always have fresh fruit (pineapple and papaya very tasty), vegetables (especially tomato and cucumber) and a diet based on rice and fried chicken every day. We supplemented each day with cold meats of all kinds, cheese, piquitos and olive oil which gave us a lot of comfort. Every night we had cold beer and carbonated drinks of all kinds in our accommodation, where dinner was brought to us. Similarly, we had a fridge at the Hospital in Dr. George’s office which was always stocked with water and soft drinks to compensate for sweat and exertion losses. Every day we were picked up by two vans at 7 a.m. and taken to a small room 50 metres from the Hospital where we were served breakfast and by 8 a.m. we were at the Hospital every day.

The working day was quite organised and each day we had 20-30 patients there who we saw little by little and filtered to indicate the surgeries for the following day, taking advantage of the time between one surgery finishing and another starting. The working days were interrupted by a 30-45 minute lunch break in Dr. George’s office and then lasted until about 10.30-11pm. Each day early in the morning we would visit the inpatients to assess for postoperative complications and discharge them.
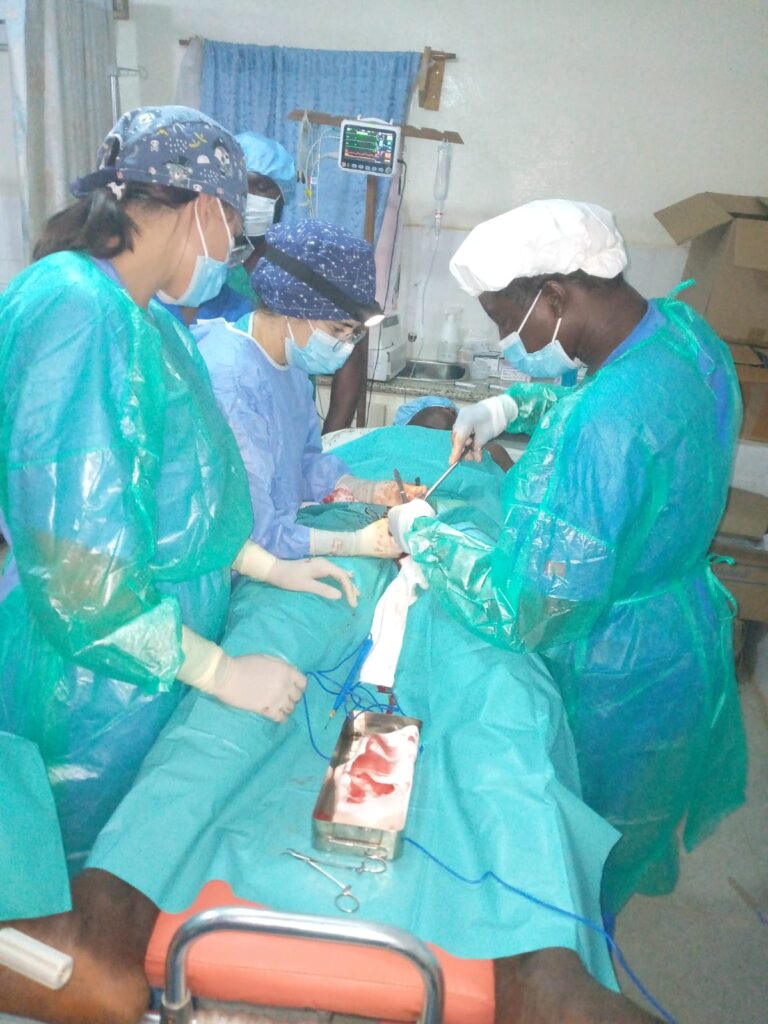
A total of 7 and a half days of work, including from Sunday 23 January at 8 a.m. until Sunday 30 January at 3 p.m., were spent. A total of 152 patients were operated on
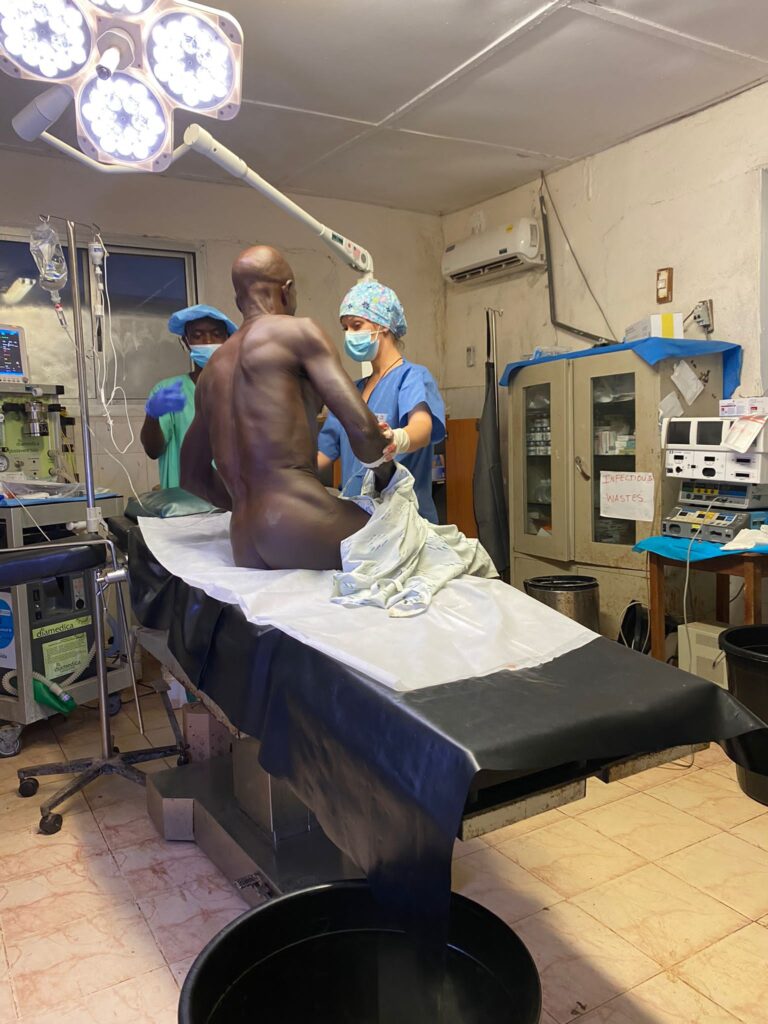
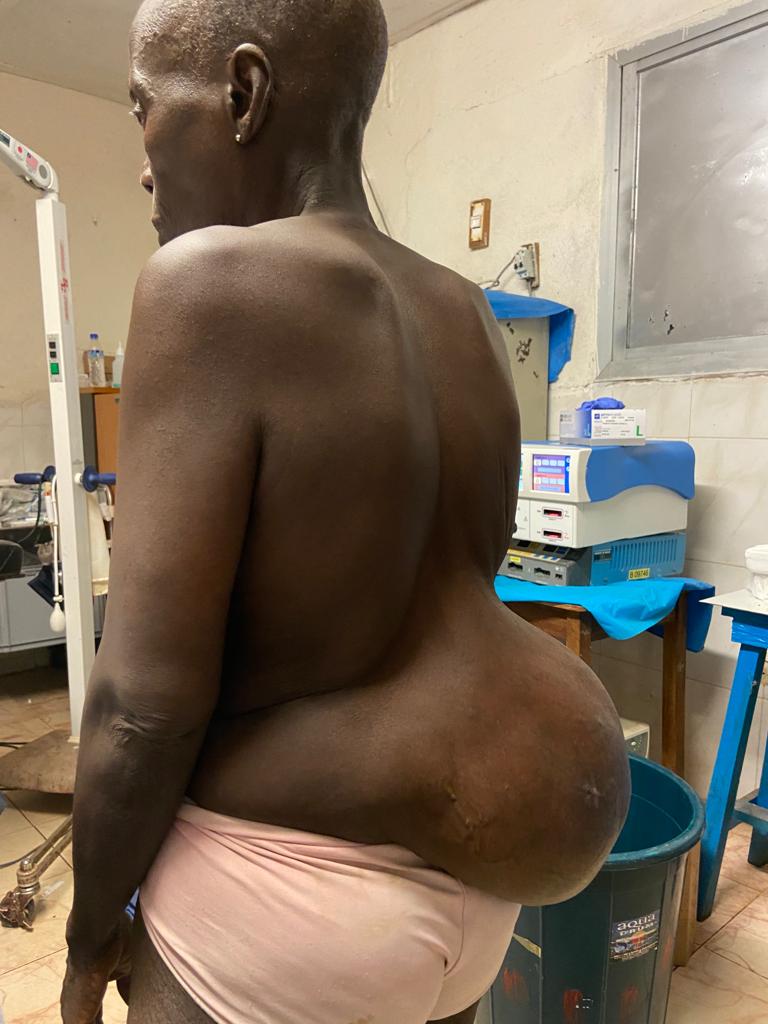
185 surgical procedures were performed, which can be grouped as follows: 109 inguinal hernioplasties (15% bilateral and another 15% reproduced); 20 umbilical / epigastric hernioplasties; three large eventrations, two of which were associated with abdominoplasty; nine giant goitres in which five total and four subtotal thyroidectomies were performed;
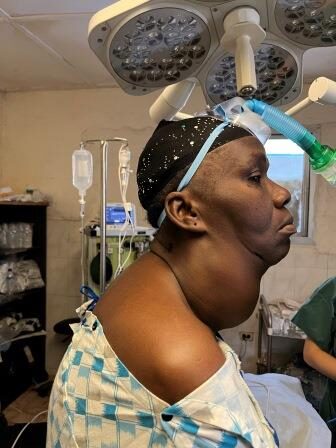
Tthree splenectomies for giant splenomegalies; ten hydroceles; five cryptorchidectomies; one orchidectomy for neoplastic neoplasia; one orchidectomy for neoplastic neoplasia; and one orchidectomy for testicular neoplasia; one radical hysterectomy and double anexectomy for giant ovarian neoplasia; one radical right nephrectomy for a 25 cm tumour dependent on the right kidney; two cord cysts; 21 minor surgeries under local anaesthesia (lipomas, sebaceous cysts, granulomas and keloids); and one hygienic surgery for the removal of a very advanced acral melanoma.
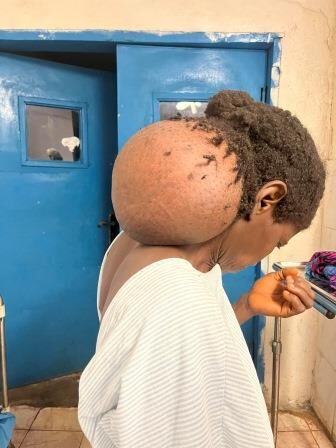
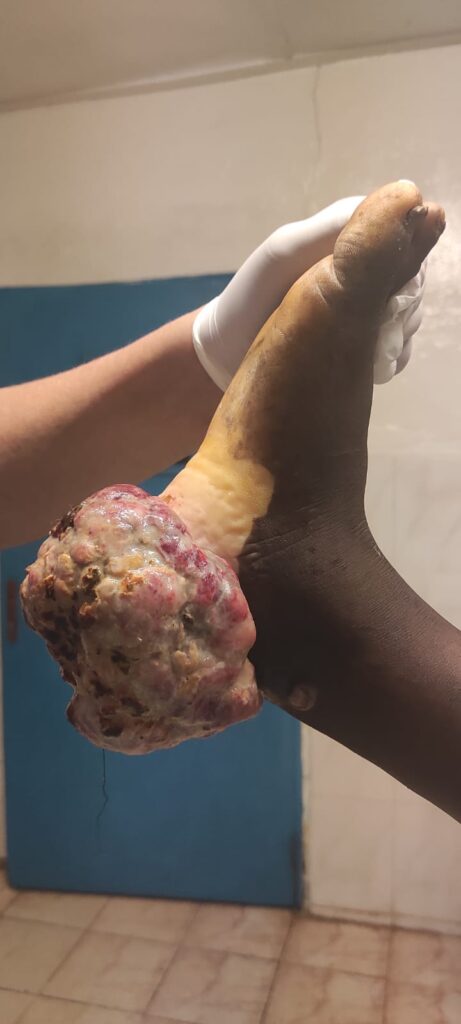
The only major complication recorded was the need to perform a temporary tracheostomy on a patient with postoperative disnoea due to paresis of both vocal cords (both recurrent nerves had been preserved and there is an imaging record). In all other surgeries we had no major or minor complications recorded. The two surgeons at Jallahlone Hospital (Dr. Dahrly and Dr. Dwanna) actively participated in the vast majority of the surgical procedures as assistants and we tried to explain as much technical knowledge as possible. The cooperation of the nursing staff, anaesthesia assistants and anaesthesia technicians at the hospital was excellent and made us feel very comfortable.
During our stay we were greeted by the major of the county of Gbarpolu and we had an audience with the senator of Bopolu, who thanked us for our presence as this was the first international team they had received and made me realise that Peter George is a very well positioned person in the eyes of the authorities and a reference point for health in the region. I would like to point out that with the sponsorship of the United Arab Emirates, a large hospital is being built in Bopolu, which is well advanced and has all kinds of services, more comfort, more space and more operating theatres. Those responsible for the work, who are Lebanese, have been very kind to us and have invited us to have lunch one day in their facilities.

To sum up, Jallahlone Hospital is a perfectly prepared site for surgical campaigns and Peter George is an influential person, with great influence among his people and great organisational skills. It is to be hoped that many more missions can be held in Bopolu in the future, especially when the new hospital is completed. Overall, it has been a very hard mission from a physical and working conditions point of view, but all members of the team have been very satisfied and satisfied with the work done and the results. The average cost per volunteer was almost 2000 Euros per person, including flights, transport by car in Liberia, food and accommodation.