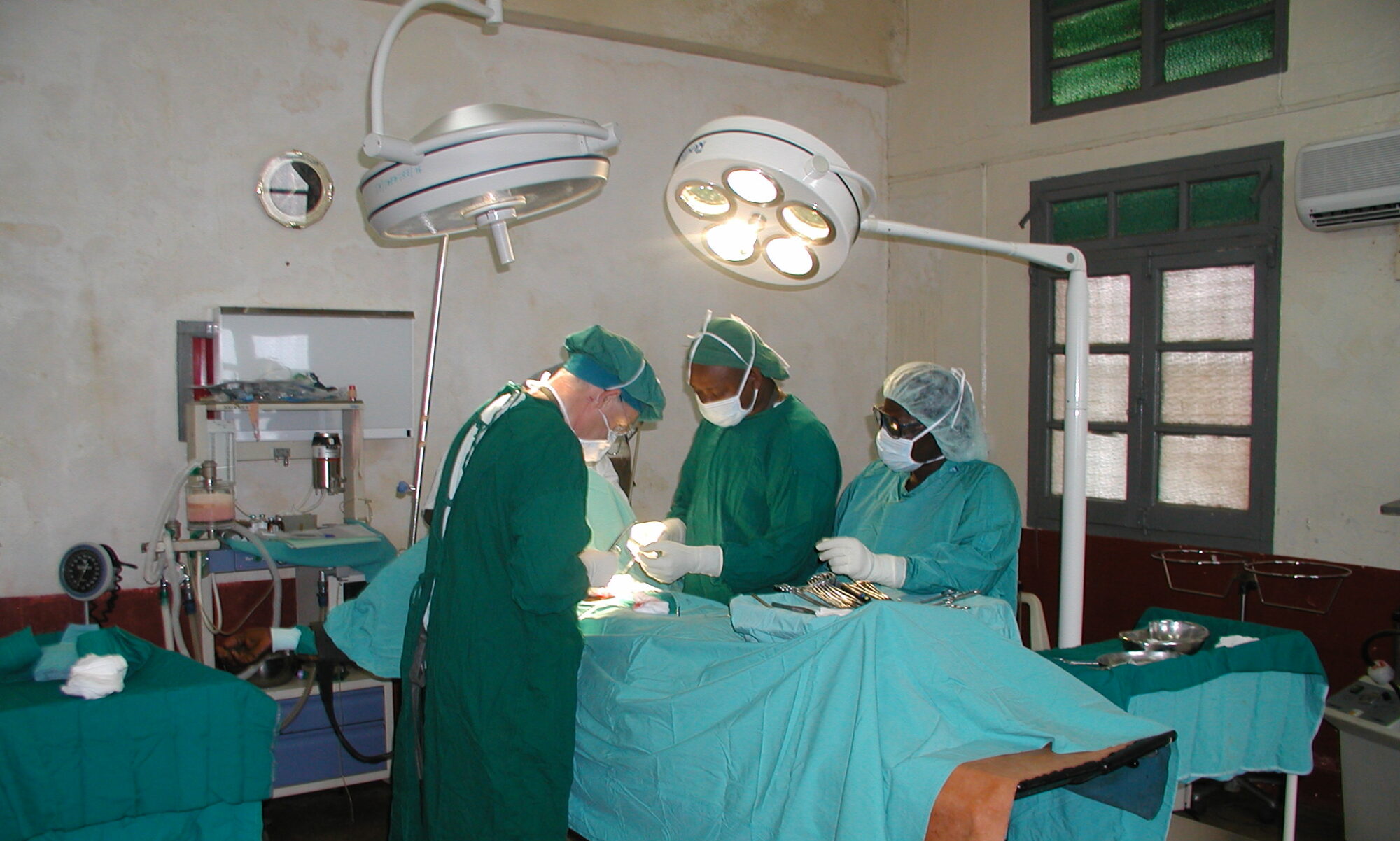
Esther and Jereline Medical Centre, Ganta City, Liberia
November 30th – December 8th 2019
This was a four surgeon Hernia International Mission:
John Hobbiss, Colorectal Surgeon, UK
Mahesh Pai, Vascular Surgeon, UK
Emma Sidebotham, Paediatric Surgeon, UK
Thorbjorn Sommer, Bariatric and Colorectal Surgeon, Denmark
John and Thorbjorn had been on previous Hernia International mission, John on the first trip to Ganta City in July 2017, a first trip for Mahesh and Emma. This was Hernia International’s 7th trip to Ganta City. We arrived together on the evening of Friday November 29th, on a flight from Brussels, being met pre passport control by Dr George, Chief Medical Officer, Esther and Jereline Koung Medical Centre.

We spent the night in Monrovia and were driven to Ganta City next morning, arriving around midday. After lunch we proceeded to the Medical Centre. Dr George had already triaged and admitted 4 paediatric patients and having unpacked our equipment we got the mission started by operating on these that afternoon.
And that was how the mission progressed so that running four theatres, over the 7 and a bit days of operating we operated on 197 patients (plus complications detailed below and the caesarean section Torbjorn assisted with!) repairing 222 hernias, predominantly inguinal, some femoral, with occasional umbilical hernia repairs and hydrocele surgery.
This was only possible due to the large number of patients Dr George had attracted to come for assessment and surgery by an excellent radio campaign to get the message out about the mission, even after a previous mission only two weeks before. Furthermore, Dr George saw all the patients in clinic, triaging them and admitting them to the wards, so that we were simply in theatres ready to operate, with only a handful of patients triaged for surgery that we then declined to operate on (e.g. umbilical hernias in infants). Getting started in the mornings sometimes felt slow but once we began, for the three adult theatres, the next patient was sitting on a chair outside the room ready and waiting to be examined and operated on. For the paediatric patients we did a ward round to assess and mark them then they were brought to theatre as soon as the one was sent back to the ward post op.
We had one anaesthetic technician/nurse between the four theatres, Emmanuel from Sunday to Wednesday with Abenego from Thursday to Saturday, and some input from a third nurse anaesthetist, Cyrus, who went from theatre to theatre giving spinals with great efficiency and efficacy, with occasional caudals and supplementary ketamine for the children.
The theatre staff were extremely helpful and many were excellent surgical assistants. Othello in the paediatric theatre was particularly helpful, doing a ward round with me, helping to translate and compiling lists of the patients for the day.

There was a local surgical trainee, Wanaka, who operated for several days with Thorbjorn who was able to train her well to perform mesh hernia repairs over the course of the mission, an excellent adjunct to the performing of surgeries. In total we lost about two days of operating spread over two of the four theatres for caesarean sections and laparotomies.
I operated on 50 children and two older teenagers but my adult colleagues humoured me and took me through 3 adult mesh hernia repairs so that I’d feel better prepared to do adult hernias if there were less children on a future mission.
We stayed in Jackie’s Guest House about 2 miles from the hospital, safe, clean air conditioned accommodation with a plentiful supply of hot water and internet access. Jackie’s has a restaurant where we ate most of our meals. It also has a small shop where we purchased drinks and snacks to take for lunch along with nuts and energy bars we had brought from home: this kept us going through the day as there was no true break for lunch and the large size of our other meals meant that we did not need more.
We left Ganta City on Sunday morning. Our flight was not till the evening so we were fortunate to meet and be entertained to lunch at the Boulevard Hotel in Monrovia, by Mr Jeremiah Koung and his associate Mr Ibrahim Hamdan, who had established the Esther and Jereline Medical Centre and donated it to the local community, giving us the opportunity to explain the purpose of our mission with Hernia International and Mr Koung to explain some of his further aspiration for improving healthcare facilities in Nimba County and throughout Liberia.

Complications:
Whilst in Ganta we also came across complications of hernia operations performed by previous Hernia International missions and cases subsequently operated on by the local team. We operated on four such cases, two of whom had an infarcted testis. It was a stark reminder that the sort of cases that we were operating upon have the potential for serious complications
Equipment:
Esther and Jereline Medical Centre are able to provide very little equipment beyond surgical instruments. UK style disposable drapes and gowns are available for surgeries performed such as caesarean sections but are not allowed to be used for the Hernia International surgeries, to the point that we were expected to provide gloves for the staff assisting us as well as for ourselves. This inevitably requires some compromise in the gowning and draping we would perform in the UK against what is adequate for some degree of asepsis and what is feasible to bring as luggage on the mission.
Essentials:
Gloves – surgeon and assisting theatre staff
Skin Prep solutions
Sutures (we thought that we were going to run out and Dr George obtained more, which we paid for, through the local pharmacy. These were Chinese manufactured, appeared to be finer than the equivalent Ethicon sutures and expensive)
Face masks
Hats
Surgical scrubs
Local anaesthetic
– bupiuvicaine for spinals (multi use stoppered vials best, even if these would be single use in UK)
– Lidocaine or bupivacaine for local infiltration/LA procedures.
Drapes
Gowns
John brought many boxes on Co-amoxiclav to be given for at least the mesh hernia repairs for 48 hours post op. We understand from the theatre staff that the patients were charged for them. We had no role in them being given out as these were taken over by Dr George when we unpacked the equipment.
One theatre of the rooms we used had an operating light, head lights were essential in all other rooms. There was sometimes a wait to get the electricity running in the morning but little interruption of the lists once running.
Alcohol for hand prep is also useful. The water ran out by the end of some days.
Expenses:
This is an expensive mission compared to many in Africa. The Liberian economy currently works largely through the US Dollar. Accommodation is Western prices: we paid $60/night in Ganta, plus paying an extra night to secure the accommodation, and $75 in Monrovia. All food is in addition to this, and again at Western prices $20-30/day, we bought snacks for lunch. Transport for the week within Liberia cost $480 for the team.
There is also the expense of equipment to bring that is greater than many Hernia International projects. We paid for 16 vials of bupivacaine, more bottles of skin prep and elastoplast tape in addition to the sutures. Bringing more prep and local anaesthetic would be helpful.
Acknowledgements:
We wish to thank the following organizations for supporting this trip
Dorothy Whitney Elmhirst Trust
BMI Beaumont Hospital, Bolton
Circle Hospital, Bath
Molholm Private Hospital
Teal Laboratory Services Limited