Benin, April 21-29, 2017
Cea-Cea Moller-team leader,
Richard Turner – surgeon and hardest worker
Christine Russell-surgeon and bold French speaker
Philip Gribble-anaesthetist and educator
Paul Scaife-surgeon and fastest runner
Clancy– teenage anaesthetic nurse student scribe scout interpreter!
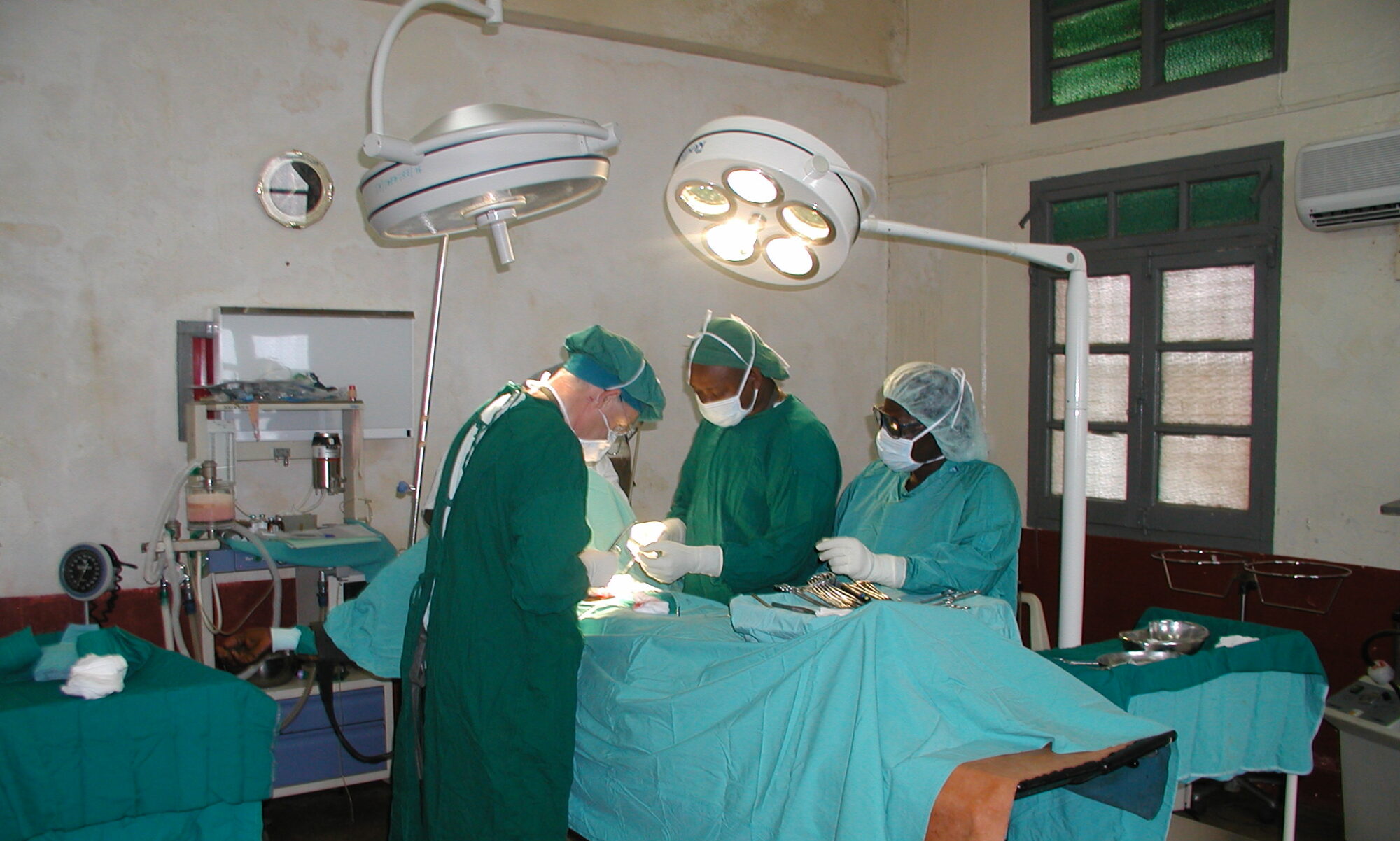
This is a small mission hospital in Dangbo that provides general medicine–adult and paediatric, maternity, an immunization and an HIV/AIDS service. It has a functioning pathology laboratory. There is a departmental hospital about half an hour away where the patients for emergency caesarian are sent. There is no full time surgical team in Dangbo, just charity missions from other countries–particularly one paediatric surgical team from Spain. This was the first mission from Hernia International.

We were 4 surgeons, 3 from Australia and 1 from the UK, 1 GP anaesthetist from Australia and 1 mission aide from Australia. Communication between us and the local staff was in French. Some patients spoke French but mostly the local staff translated for the patients between French and Fon.
During the week we had a visitor from Porto Novo, a training surgeon, Dr Juste. He had been a general practitioner at the hospital in Dangbo and often assisted visiting surgical teams. He had thus been inspired to enter surgical training. He recounted that surgical training was a very expensive exercise and that his parents had to support him financially. When he qualified he said that he would find it difficult to come back to Dangbo to operate because the patients would not be able to pay him. In the hospital in Porto Novo they did not do mesh repairs of inguinal herniae but performed a Shouldice repaire
Pre-arrival
Yellow fever vaccination and a visa are required to visit Benin. The 4 Australians needed to send their passports to London to obtain the visa. The process of returning the passports to Australia was somewhat precarious!
It is difficult for the hospital director Sister Opportune, to communicate by e-mail. She finds ‘WhatsApp’ to be more efficient when arrangements are being made for the missions.
Arrival
At Addis Ababa airport extensive questions were asked about the goods we were bringing in but the Hernia International introduction letter, the itemized list of contents plus the fact that we were only staying overnight meant we were allowed through. At Cotonou airport we were also questioned about the goods but the mission authority paperwork from the local health directorate in French was enough to allow us in the country with the donated medical supplies.
One of the nuns and a driver met us at the airport in the hospital ambulance/bus. The drive to the hospital lasted just under an hour over very potholed roads with dense traffic and the impression of many near misses!
Accommodation
We stayed about a 500m walk from the hospital down a dirt road in a paved compound of 2 large buildings, the use of which is donated by the owner who lived in Porto-Novo. This was luxury compared to the local population’s housing. Each of our 3 large rooms was air conditioned with an en-suite. Cold drinks, including beer, were supplied in an insulated box with ice added occasionally. Bottled water was provided. No bedding or towels were provided.
There was no access to internet other than by walking to the local hotel (about 1km away) to use their Wi-Fi. For the Australians, no phone coverage was possible. Our English surgeon Paul was able to get somewhat intermittent coverage.

Food
Breakfast, lunch and dinner were provided by the nuns in their dining room at 5 minutes walk from the operating theatre. It was delicious, with either an African or a French focus. We ended up cutting back on lunch and snacking in the theatre store room so we could get our programmed work finished.
Patient Preparation
In preparation for the visiting teams, advertising is in the form of word-of-mouth, through the church network, radio commercials, through family and friends and even a man on a bike riding around with a megaphone informing the community at large. The patients write their name with their problem and contact details down in a book at the hospital pharmacy. The prospective patients are then vetted by the local doctors before being seen by the team.
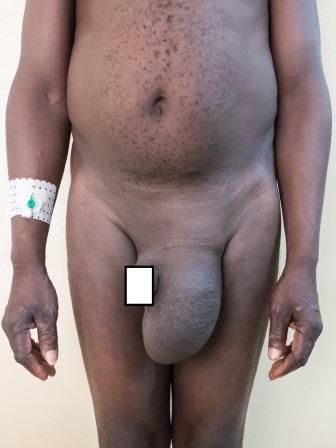
Surgeon Richard flew in from Australia, arriving Friday night, and on the Saturday saw 100 patients who needed surgery. He programmed 10 patients each day for the Monday to Friday that we were to be operating. There were 45 inguinal herniae (2 bilateral), 1 large incisional hernia, 1 large neck keloid scar and 5 other minor procedures.
Each patient had routine bloods including HIV status pre-op. Only 1 of the 50 patients was HIV positive.

Theatre
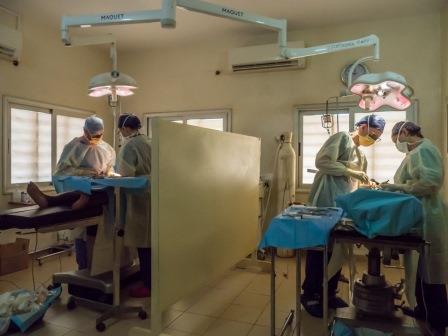
The theatre is a fairly small room (approx. 5 x 5m), with 2 operating tables, separated by a wooden screen. Thankfully it is air-conditioned! When we walked out of theatre during the day it felt like walking into an oven!
There is no pre-anaesthetic or recovery area; the patients return to a post-op ward which is in the adjacent building. For the week, this post-op ward was staffed by Gabin, a surgical nurse who came from Porto-Novo for this purpose and even slept in the ward for immediate access to the patients. He had some help from a nurse assistant.
Oxygen is provided by a large cylinder. Suction is a stand-alone ‘Medpap’ machine with foot pedal; for both surgical and anaesthetic use. There is a Drager ‘Fabiusplus’ machine which can provide ventilation (VC & Manual Spont. only) along with a monitor providing a screen with readout for SpO2. No airway gas monitoring is available. Both paediatric and adult circuits are present with spares. A ‘Laerdal’ bag is also present. Oxygen tubing, connections, ETT tubes, iGels & LMAs are also available, numbering in the 10s for each (inc. paediatric). At least 4 intubating stylets and 4 Cook’s-brand bougies were available. IV access was well supplied with cannulae ranging from 14 – 22g. There was a large number of various spinal needles (20 – 27g) along with 5 central line kits.
Presumably left-overs from previous teams, there was a surprisingly wide variety of drugs available, although many ampoules were out of date. IV drugs we found on arrival included :
| AdenosineAdrenalineAlbumen 20%AmiodaroneAmpicillinAtropineBupivacaineBuscopanCa ChlorideCalcitriol | CeftriaxoneClindamycinDiazepamEtomidateFentanylFlumazenilFrusemideGentamicinHaloperidolHydralazine | KetamineLignocaineMetaclopramideMetronidazoleMidazolamMorphineNaloxoneNeostigmineNitroprusside | OndansetronPolaraminePropofolRocuroniumSteroids (5 types)SuggamadexSuxamethoniumThiopentoneTranexamic Acid |
In the store room was an eclectic array of equipment, ranging from a multitude of sterile gloves and dressings to a variety of instruments and even an old portable U/S machine. Suture material and small disposable drapes seemed reasonably plentiful.
Operating gowns were limited in number; for most operations yellow infection control gowns were used. We had brought only 30ml syringes. Small syringes were not abundant, making measurement of small volumes difficult (e.g. when mixing adrenaline in to LA). Another surprising deficit was in small stainless steel gallipots for mixing. The array of instruments is generally adequate, the most prevalent issue being the blunt dissecting scissors; bringing sharp scissors would have made a material difference to the operating.
Sterilisation is done on site with a turn-around time of approximately 45 min. It was unusual for us to have to wait for this.
Sister Ruffine was an able scout nurse in theatre. She managed the pace of the patient flow related to sterilized trays being available and laying out the next sterile set up for each patient.
Power was generally reliable, although it was not unusual to have brief outages (for 2-3 minutes) throughout the day. The main inconvenience was waiting for the diathermy to re-boot. Fortunately, this had no effect on the air-conditioning. Whilst we had brought head-torches as a fallback, these were rarely used.
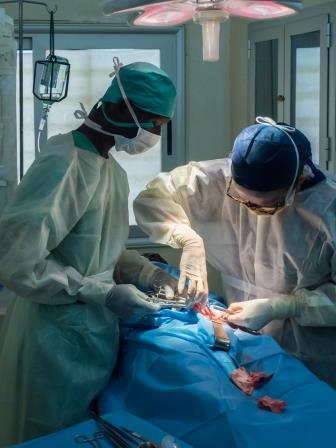
The operating lights are of reasonable quality and reliable; spare globes were available and we did use one.
Each day commenced at 8:30, although the first patient usually arrived at about 9. Operating was divided between the two beds; ‘1’ being next to the anaesthetic machine. Cases were planned with the potentially more complicated ones being for bed 1 although spinals were available for bed 2 if required.
Scrubbing is at a simple sink with Chlorhexidine and alcohol; the tap is a simple knob i.e. not able to operated once scrubbed.
Operations
Local protocol outlines every patient receives IV Ampicillin 1gm, Metronidazole 500mg, Gentamicin 80mg & Diclofenac 75mg. This is continued for 24 hours post op. A glass bottle of IV fluid also comes with each patient in their small cardboard box.
Each table was manned by 2 surgeons with 1 operating and 1 assisting. This was ideal given the very scarred cases that we found. Gabin the ward nurse was an enthusiastic surgical assistant on the occasion when we were down to 3 surgeons instead of 4. Half of the patients had large herniae but even the smaller reducible cases had a surprising amount of scarring at the external ring and of the sac to the cord.
We programmed 10 patients per day and didn’t finish until 8 or 9 at night.
Anaesthetics
Spinals were required for 50% of cases. These were generally reliable although 3 men had bony obstruction; 5 required supplemental sedation and on 2 occasions, the operations exceeded the duration of the spinal. Only one patient required Ephedrine for hypotension (asymptomatic; given out of caution, especially due to Phil’s concern about the accuracy of the sphygmomanometer, rather than physiological sequelae).
Our impression was that slightly larger volumes of ‘heavy’ Bupivacaine 0.5% were needed for the spinal anaesthesia for good effect. The usual dose would have been around 2.8ml; here, easily 3.2 – 3.4ml was needed.
Sedation was primarily with Ketamine but supplies of this were limited (over half of the stock found on arrival was out of date). Fortunately, the alternative of Midazolam and Fentanyl was available. Propofol was used twice, again, from found stock.
Due to lack of gas monitoring, no recovery ward or dedicated nursing staff, as well as intermittent unreliability of the oximeter, the decision was made to avoid GA with paralysis. Sevoflurane was the inhaled agent available, no NO2 or air mix was possible, so GAs were managed on 100% O2. Two GAs were given (in both cases secondary to failed spinal insertion), both on LMA without mishap. Recovery occurred in the theatre unit until both were clearly responsive to voice alone. Oxygen was used sparingly for events of demonstrated reduced saturations <94%. Post-op analgesia and management was done by Gabin, the surgical nurse in the post-op ward. It appeared that the range of analgesia extended to oral agents and IV Diclofenac. As such, all patients were given either local infiltration of 0.5% Bupivacaine or TAP blocks at the end of the operation (including patients with spinals).
Post-Op
The expectation by local staff was that all patients would go home the following day. The ward is essentially a large room with closely spaced beds. It was notably hot and humid with the only medical facilities apparent being the IV flask holder and a sphygmomanometer.
Close assessment of post-op pain was not possible secondary to the language barrier but patients greeted us with smiles and waves, so the assumption was that the experience was within their expectations. The patients, in French or in Fon, when they got the chance thanked us and said “God bless you”.
Student Participation
15 year old Clancy accompanied her mother Cea-Cea on this trip as mission aide. Her participation was vital to the smooth running of the mission. She took primary responsibility for documentation of the team’s activity. She also proved adept in performing as a de-facto anaesthetic and scout nurse as well as in some English/French translating.
Suggestions for next time
Surgical
* Program 8 patients per day
* Theatre nurse volunteer
* Good scissors
* Sterile gowns
* A new diathermy machine – one of the 2 didn’t seem to be working very well
* Diathermy handles and blades
* Scrotal supports
* Gallipots
* Self retaining retractors
* Large sterile drapes that cover the whole patient
* Local anaesthetic
* 2nd Mayo instrument trolley
Anaesthetic
* Oximeter, BP, capnography
* Small syringes for mixing
* Large non-sterile gloves for Phil
* Laryngoscope
* Portable U/S
Other
* Theatre snacks!
* Room shelving for storeroom
* Clear plastic organizing boxes
* No-touch tap to install for scrubbing (and plumber!)
Overall we had a wonderful time and I would recommend this mission to anyone with a sense of adventure and some heat tolerance. At least one French speaker per mission would be ideal. Cea-Cea loved the African “tissu wax” fabrics the locals wore. The staff arranged for a local woman to display some samples so she could buy some to take home at a very cheap price. We all left very quickly after the last operating day so unfortunately we could not do the sightseeing trip to the river that Sister Opportune had planned for us. Next time!
Cea-Cea Moller
Team Leader