REPORT BISHOP MURRAY MEDICAL CENTER, MAKURDI, NIGERIA
DATE 09-05/18-05 2025
Contents
1. TECHNICAL REPORT: 1
2. CAMPAIGN REPORT 1
3. CONCLUSION 2
4. BUDGET: (small breakdown of expenditure) 2
5. SIGNATURES 2
1. TECHNICAL REPORT:
1.1 DATES AND LOGISTICS DEPLOYED:
We started the trip on the morning of 09/05. 2 members of the group left from Vigo, 2 from Gran Canaria, 1 from Granada and we met up in Madrid with another 4 members of the team to take the flight to Doha. There we meet up with the last 2 members of the team, who leave from Barcelona. In total 11 people take the next flight to Abuja.
We buy the plane tickets through Angelis, an agent of Halcon Viajes.
To enter the country it is necessary to obtain a visa, which has been a terribly complicated procedure and has caused us a lot of problems. First you have to fill in an online form and pay 258 dollars. Then you have to bring to the embassy in Madrid your passports, proof of payment, 2 photos of each of you, an individual letter of invitation from the bishop of the diocese of Makurdi and a copy of the bishop’s passport. It should be taken into account for future missions, if any of the members of the group have a trip for which they need the passport in the weeks prior to the campaign (as happened this time with 2 members of the group), as you know when you hand in the passports, but not when they will be returned to you. We were fortunate to have the help of Yaili, a contact who helped us in the previous mission, to get these passports in time. Thanks to Damian and his great patience, as he went to the embassy 6 times and spent the whole morning there, we got the last visa 1 week before departure. We also had to pay for one of the visas twice, due to a logistical problem, apparently impossible to solve without filling in a new online form.
This campaign is carried out in collaboration with Hernia International, although in this case all the participants are volunteers from Surgeons in Action (Cirujanos en Acción). The campaign was coordinated with Dr Austin Ella, Associate Director Program Management at the Catholic Caritas Foundation Building and Dr Thaddeus Aende, a physician at Bishop Murray Medical Center.

1.1 ADULT PATIENTS:
Number of patients: 89
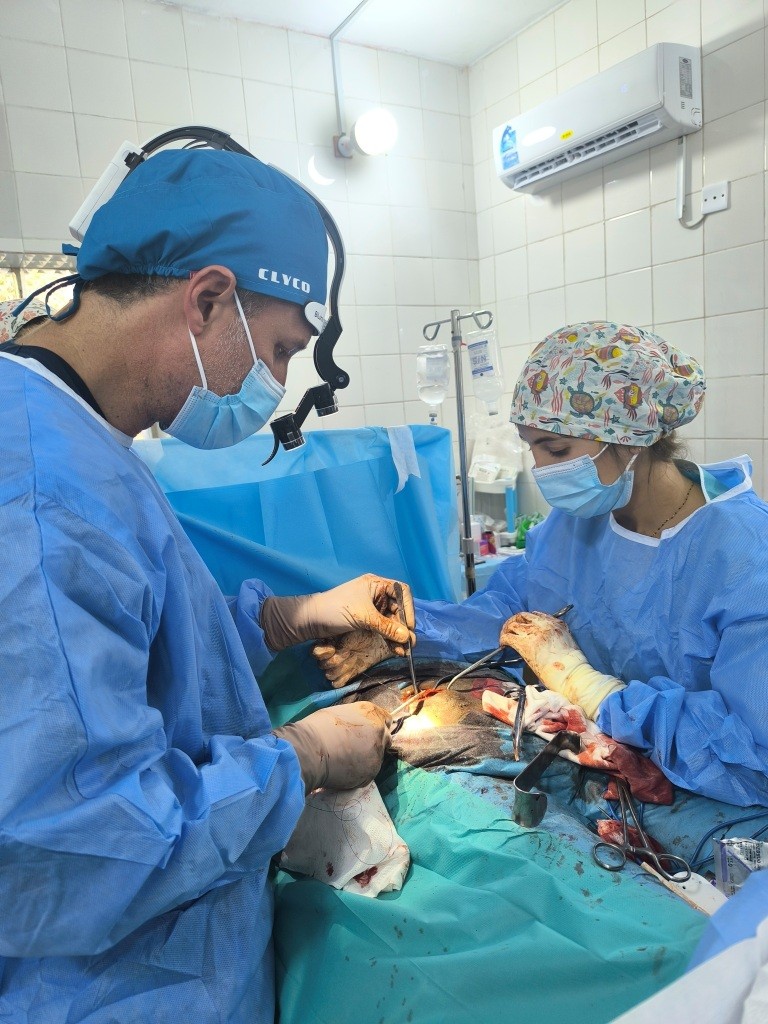
Mostly abdominal wall pathology, goitres, hydroceles and large lipomas were operated on.

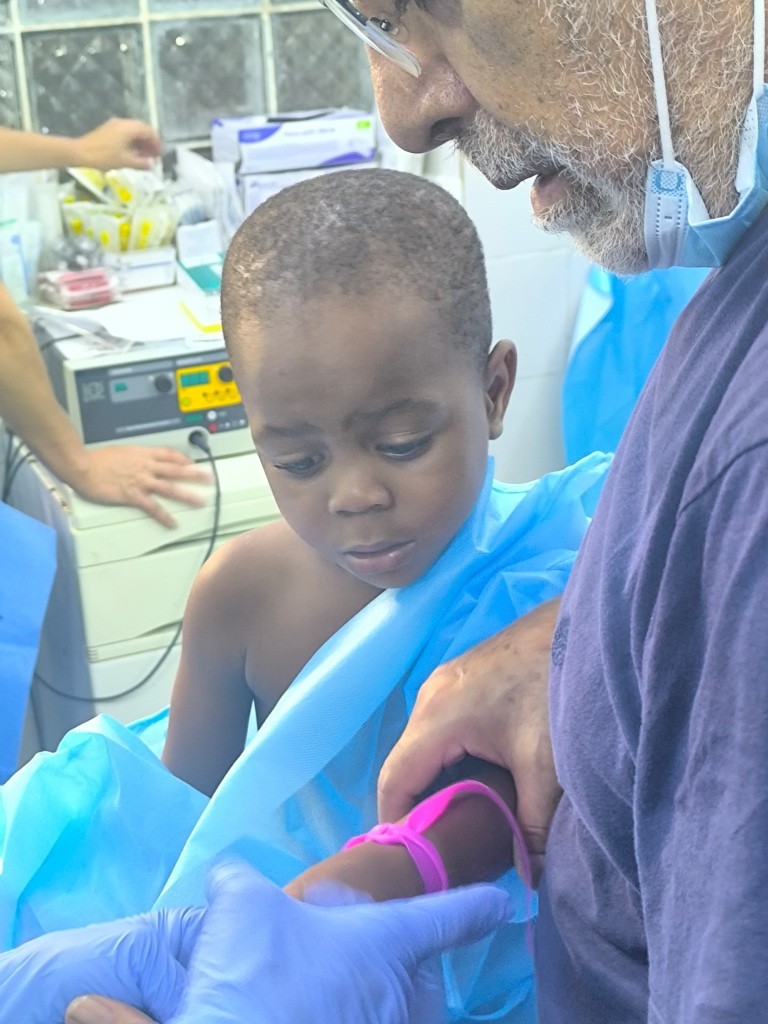
1.2 PAEDIATRIC PATIENTS:
Number of patients: 20
Inguinal hernias, umbilical hernias and hydroceles were operated on.

1.3 Total procedures
135 procedures + 3 caesarean sections in which anaesthesia was performed.
Adults: 106 procedures
Goitres: 8 total thyroidectomies, 23 haemithyroidectomies, 1 thyroglossal cyst.
Inguinal hernia: 35 unilateral, 6 bilateral. All were repaired with the Lichtenstein technique
Epigastric hernia: 6
Umbilical hernia: 4
Femoral hernia: 3
Hydrocele: 2
Lipomas: 8
Incisional hernia: 1
Testicular tumour: 1
Reinterventions: 2
Children: 29 procedures
Unilateral inguinal hernia: 11; bilateral: 3
Umbilical hernia: 9
Hydroceles: 2
Epigastric hernia: 1
1.4 Total patients
109 patients

1.5 COMPLICATIONS:
As complications, 2 patients required immediate postoperative reoperation: 1 haematoma in an inguinoscrotal hernia and 1 bleeding in the immediate postoperative period of a total thyroidectomy. All complications resolved without further incident.
To date, one month after our return, we have not been informed of any incident.

2. REPORT OF THE CAMP
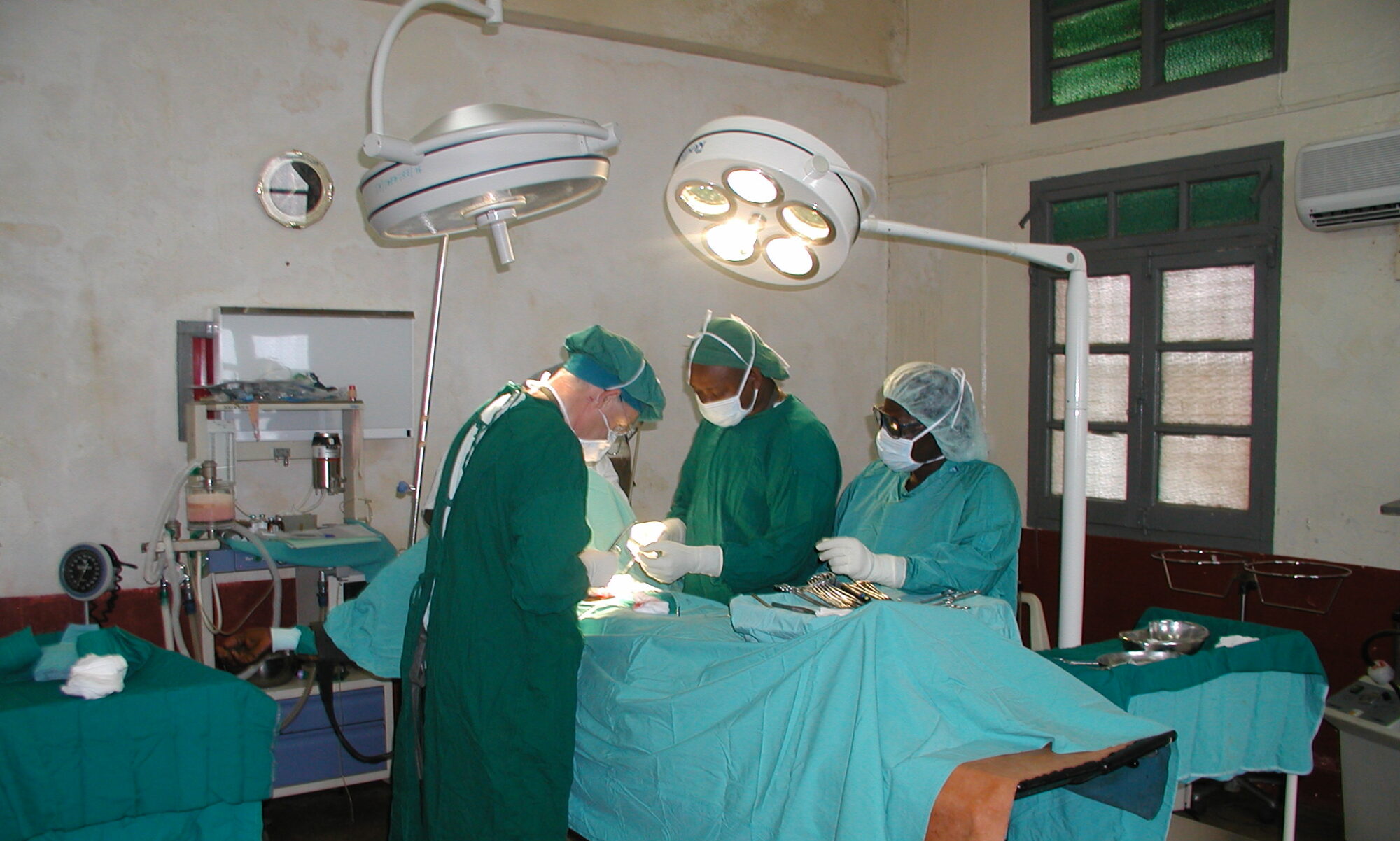
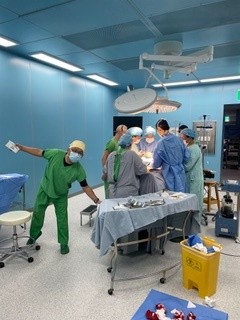
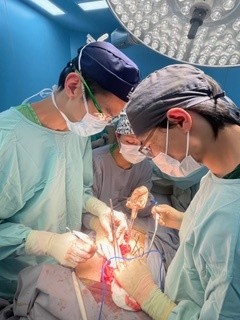
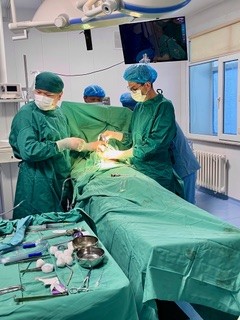
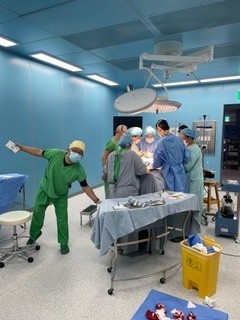
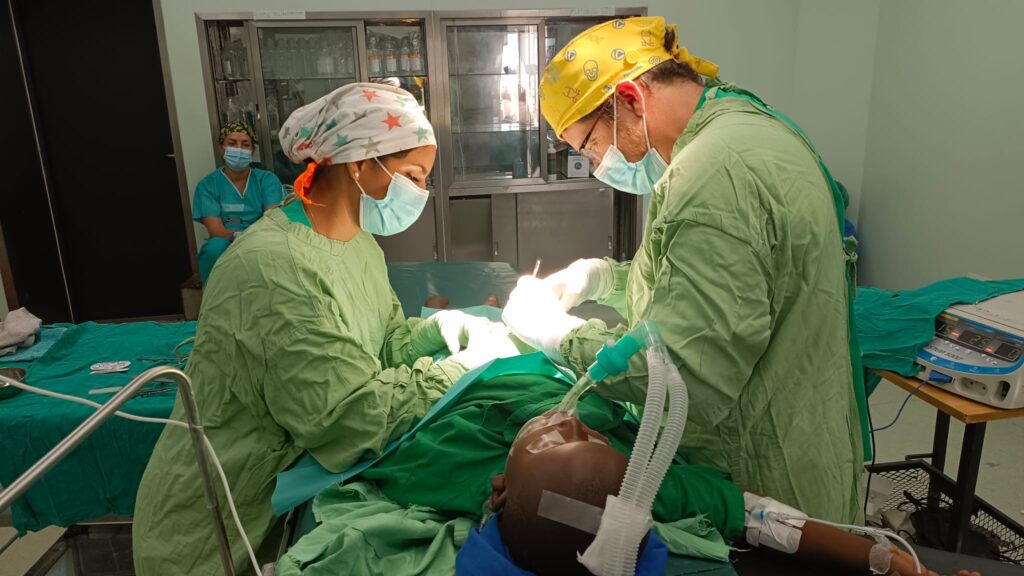
2.1. THE PLACE
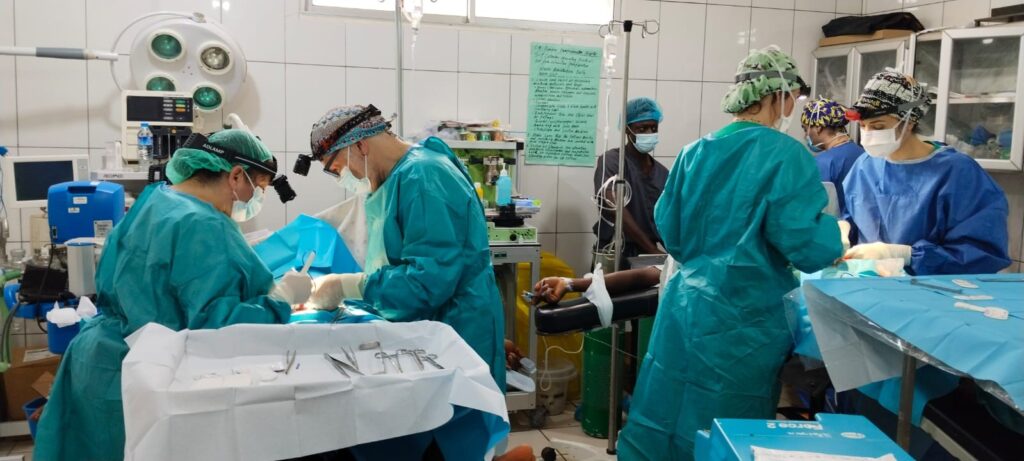
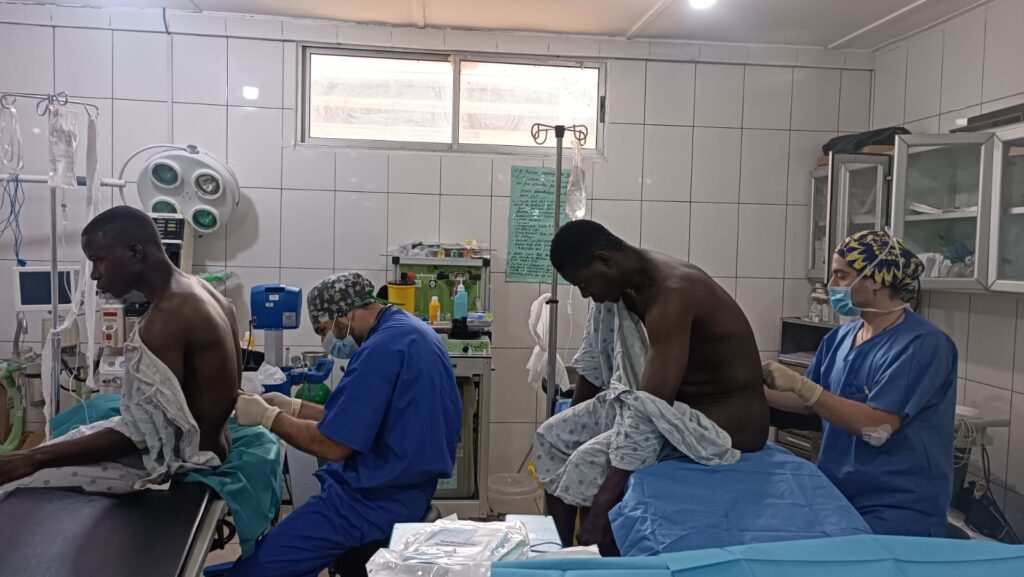
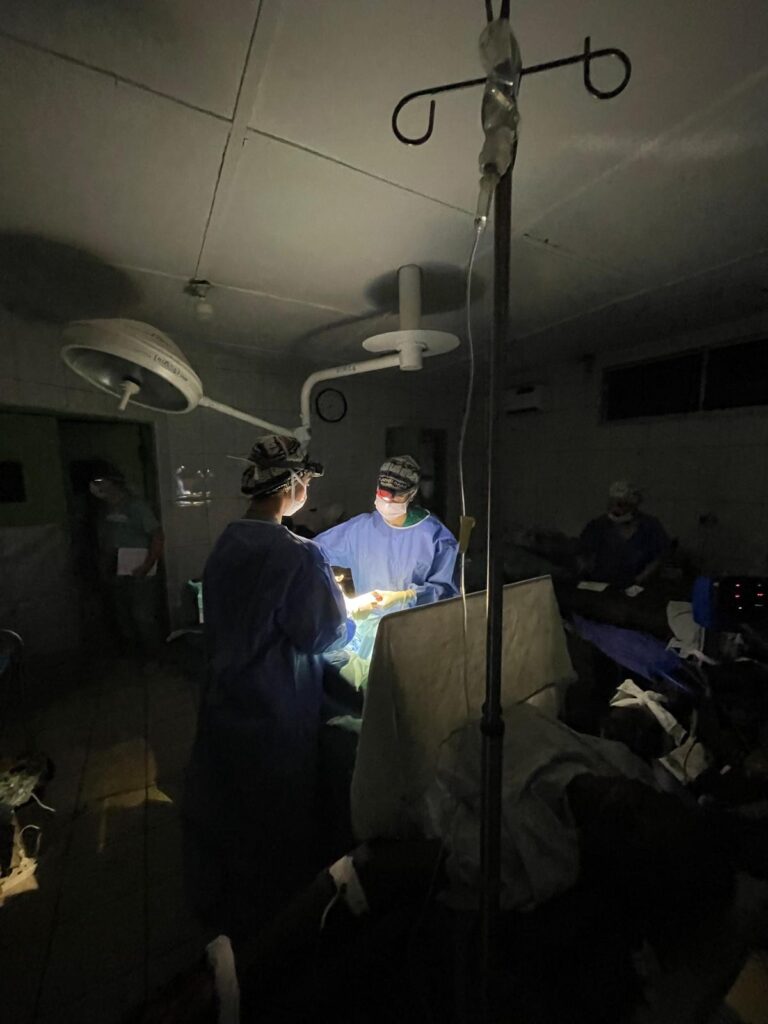
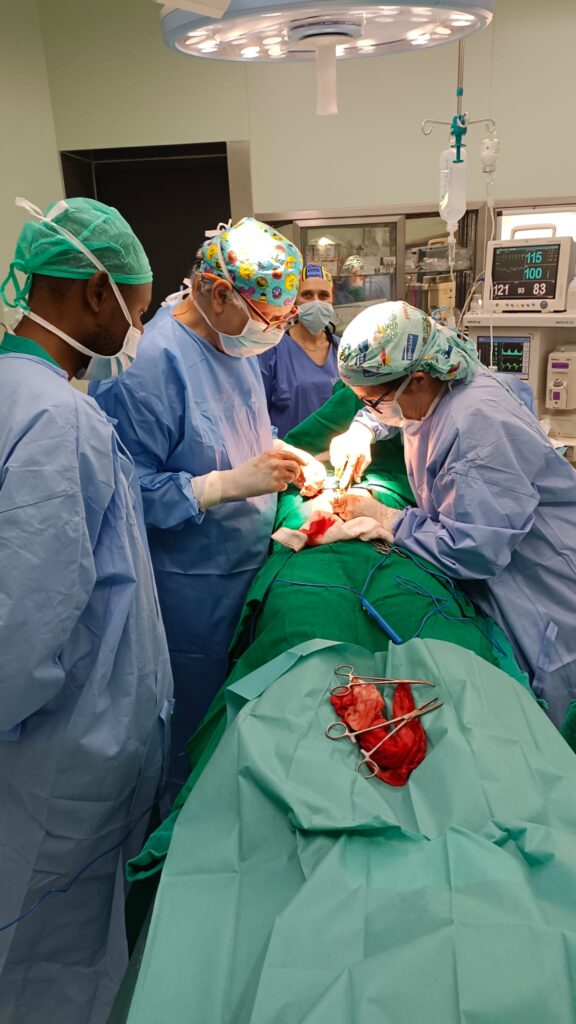
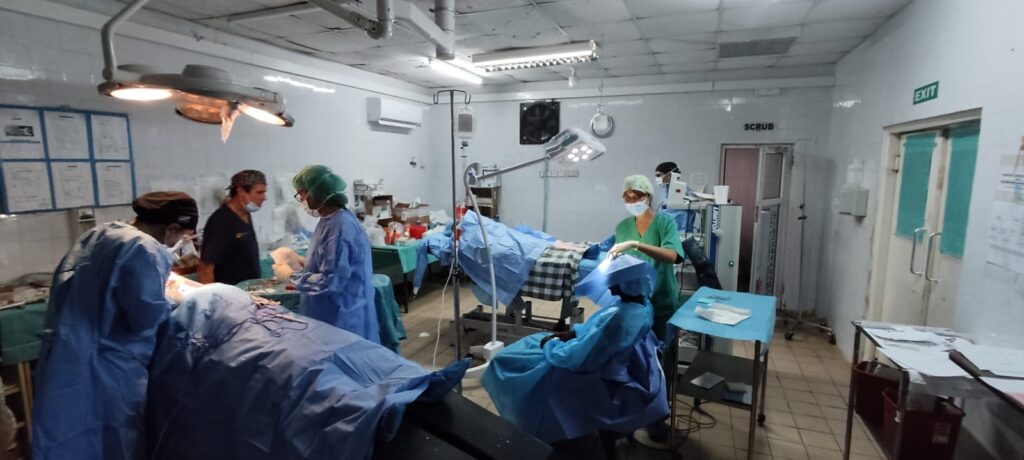
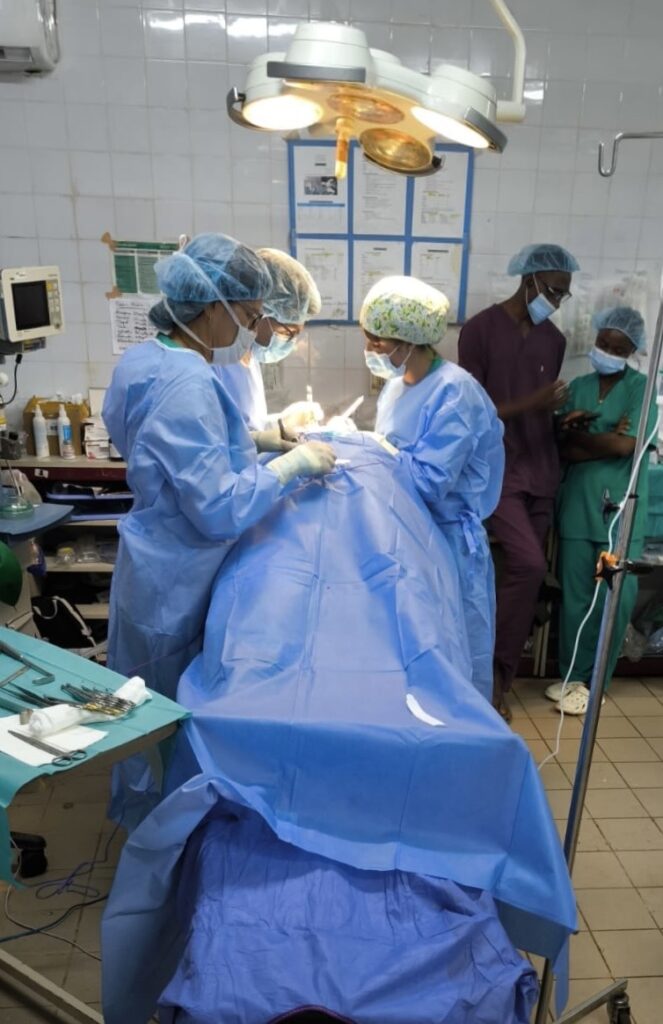
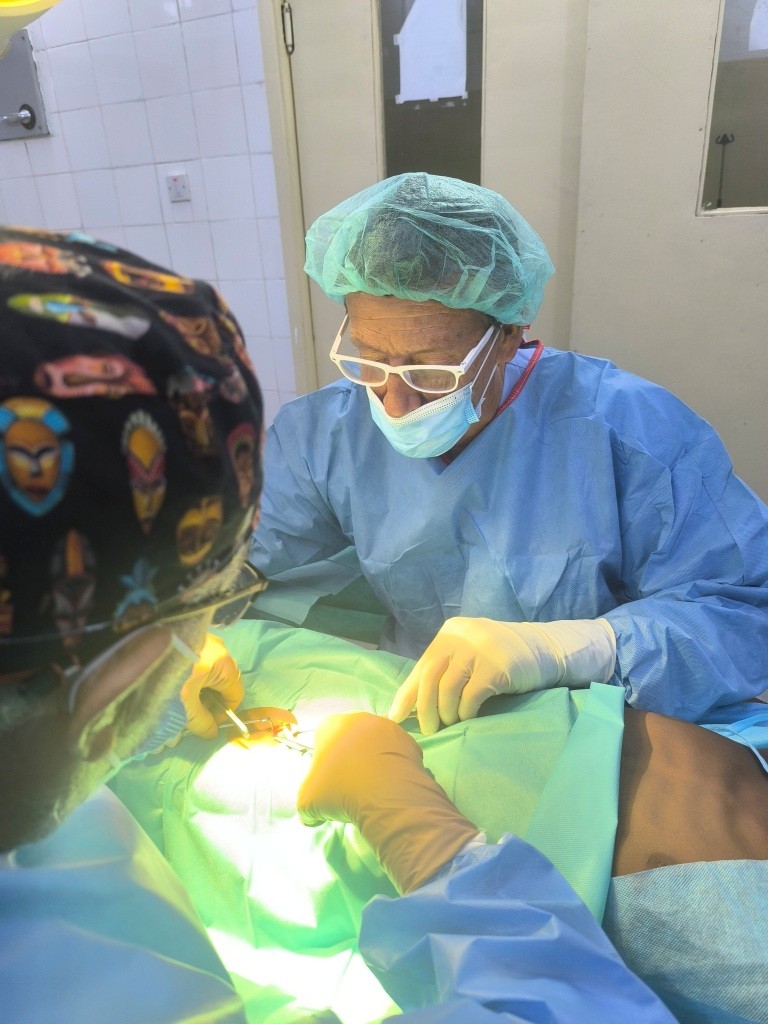
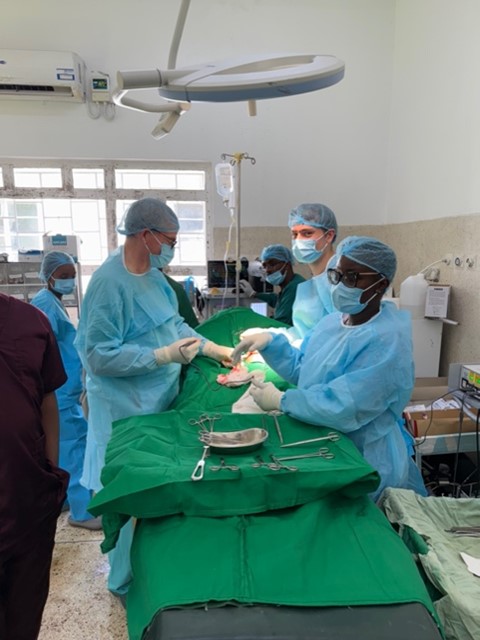
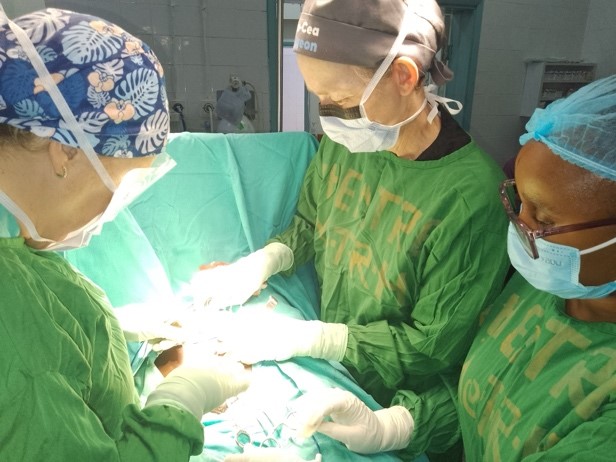
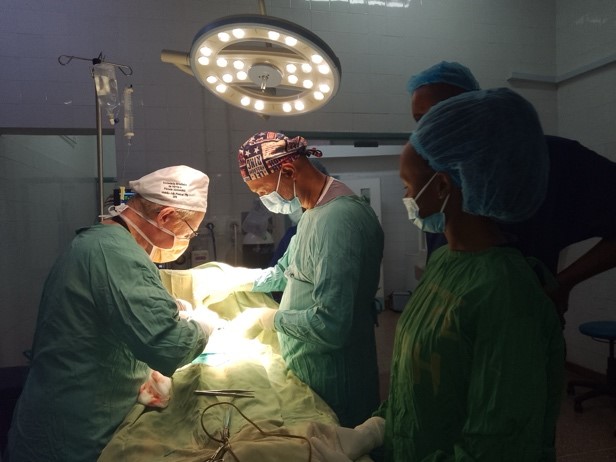
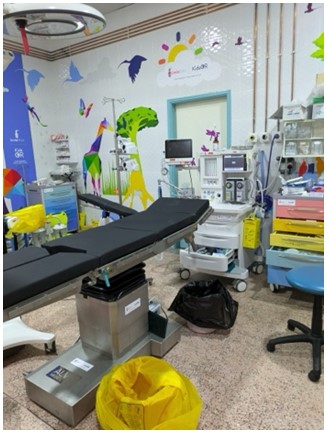
The hospital has a large operating theatre with 3 tables, which allows 3 patients to be operated on at the same time, with a screen between each table. The room is air-conditioned, which is appreciated in view of the high temperatures during the day. There are lamps on each of the tables, but they are insufficient for the surgeries, so it is essential to bring a front light. We had some power cuts, but not for long.

Next to the surgical room is the sterilisation room. On the other side is a small room where we did the recovery of patients under general anaesthesia.
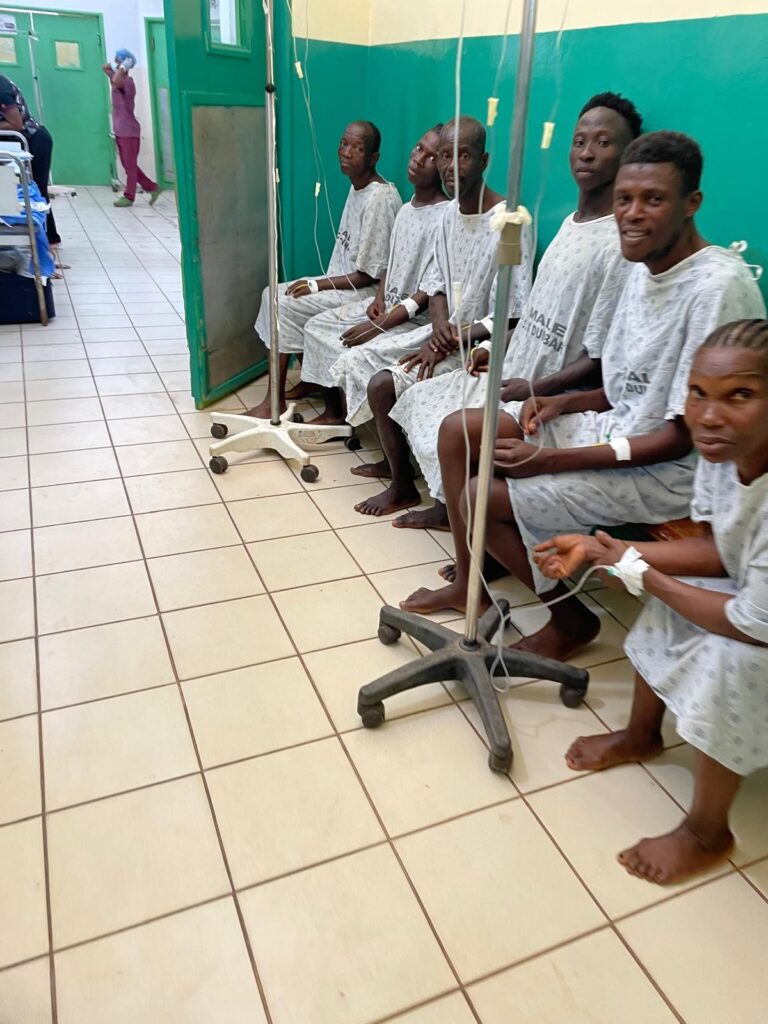
There are several separate rooms for men, women and children. They are large rooms with many beds, where the heat during the day is very intense. In addition, in one wing of the hospital, there are single rooms with air-conditioning, very comfortable for patients who can afford them, but with the disadvantage that they are not adequately monitored by the staff.
They have a laboratory where they do tests, microbiology cultures and even have a small blood bank.
The accommodation is about 15 minutes away by car. It is a residence of the diocese where we stayed free of charge. The rooms are simple, with a big bed and a bathroom with WC, washbasin and a shower (with buckets of water). There is air-conditioning, but at night they turn off the generator around 12 o’clock, until 7 o’clock. There is no wifi in the residence. In the hospital there is wifi in the dining room area, although not very powerful. Some of the team members used e-sim, although not all of them worked properly. Dr Thaddeus got us some Nigerian sim cards which also worked irregularly, but it was enough for us to communicate with our families without problems. These cards are also available at Abuja airport.
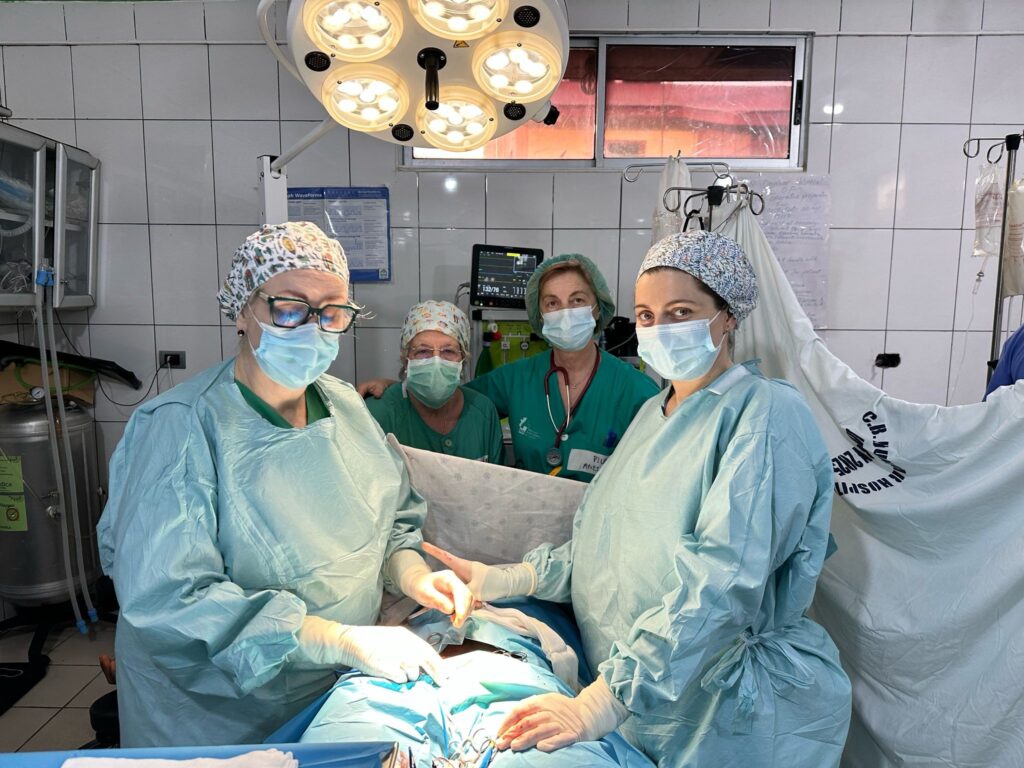
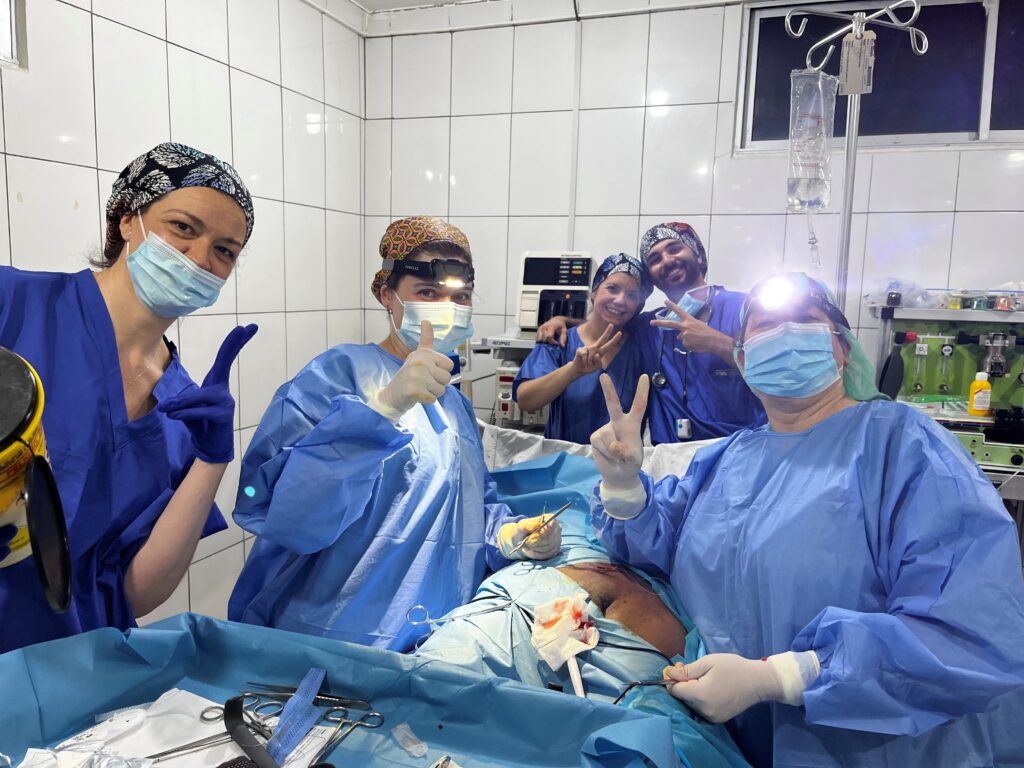
2.2. THE TEAM
General Surgeons:
Ana María Gay Fernández
David Fernández Luengas
Cristina Roque Castellanos
Natalia Afonso Luis
Salifou Hankouraou
Urologist: Francisco Enrique Valle García de la Guardia
Anaesthetists:
Rocío Díez Munar
Adrián Martínez López
Irene Macía Tejada

Nurses:
Nuria Agulló Sánchez
Paula Salgueiro Alonso
Guadalupe Martí Farre
2.3. LOCAL STAFF
Dr Thaddeus Aende, a doctor with surgical training, screened patients prior to our arrival, and during our stay we had his assistance in some surgeries.

Benedicta, an anaesthesia technician, was with us throughout the campaign, helping and showing a lot of interest in learning.
We had the help of Lawrence, Nicholas, Jacob and Slim among others, for patient transfer and organisation.
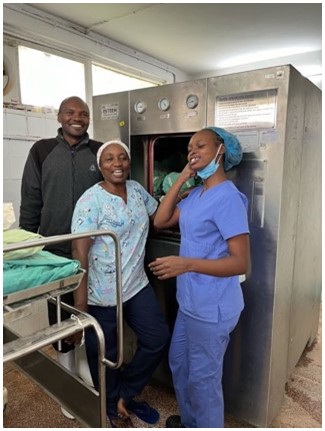
Charity and Agnes, tireless workers, took care of sterilisation and cleaning of equipment.
Father Peter, the health coordinator for the area, looked after us throughout the campaign.
2.4. EQUIPMENT
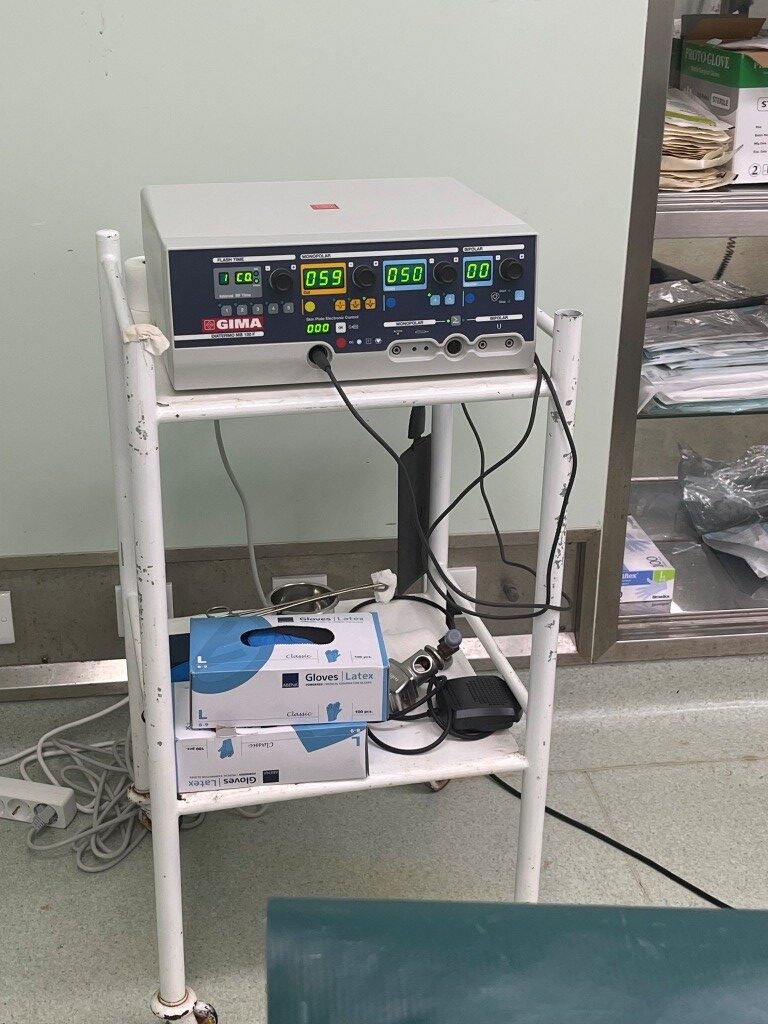
The operating theatre is equipped with:
– 2 diathemy generators donated by Hernia International and Bisturí Solidario, which work properly. We took with us 1 Ligasure generator with diathermy genertor from the foundation and another diathemy generator that was not necessary to use.
– Autoclave for sterilisation.
– Dragger ventilator model Atlan 300 with Philips monitor, donated by the César Ramírez Foundation (Bisturí Solidario) in the previous campaign, which is still in good condition.
– Surgical material: there is some surgical material there, although it is scarce and deficient, so we take several boxes of instruments from the foundation.
– Sterile clothing: they have gowns and cloth cloths, which we have not used, as the surgical rhythm of the campaign requires priority to be given to the sterilisation of material.
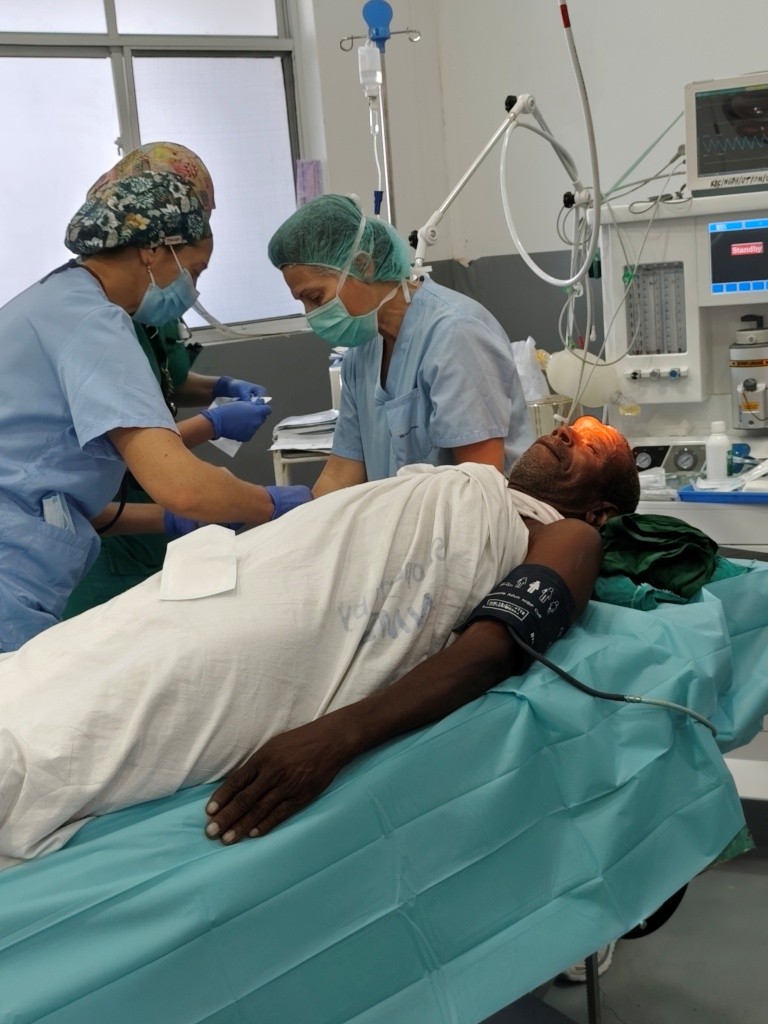
2.5. ANAESTHESIA
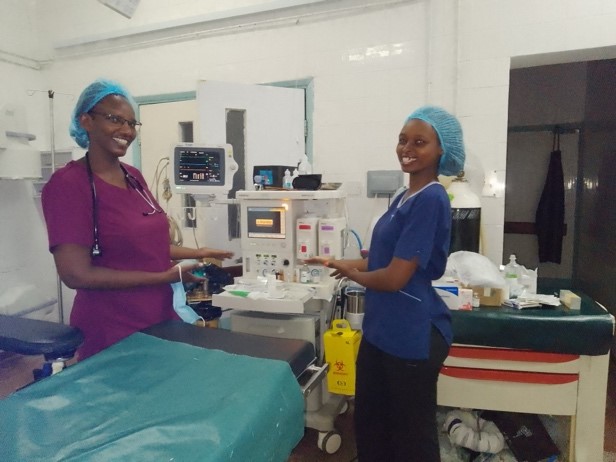
The facility has 1 Drager ventilator, model Atlan 300 with Philips monitor. The ventilator has the capacity to ventilate in Manual, VM, PC and PS, as well as an external flow system where a Mapelson can be adapted for both adults and children. It has a Cal soda system, which does not change colour and is changed by emptying and refilling the same canister; the hospital has a system to do this. The monitoring of the respiratory system consists of flows, volumes and most importantly, Capnography and inhaled and exhaled gases. The Philips monitor has EKG, PANI, Respiratory Rate and optional Temperature. There are 3 sizes of blood pressure cuff.
The ventilator is plugged into the wall with oxygen and medical air intakes, because the 2 bottles on the back of the building are for oxygen, so you only ventilate with 02 at 100%, but at very low flows. If you remove the Cal soda, this ventilator has the ability to take ambient air and mix it with your oxygen, lowering the FiO2 you give to the patient.
The ventilator also has 1 Sevorane and 1 Isoflorane vaporiser, both from Baxter.
For the other 2 OR tables there is no monitor available, but there is another oxygen bullet and a concentrator in poor condition.
We used the anaesthesia machine for the thyroidectomies, which we performed with Propofol in continuous perfusion (we carried a pump). Four of the 30 patients were intubated with a video laryngoscope, although without major complications. It should be noted that there was no laryngoscope, both the Macintosht and the airtraq were carried by us.
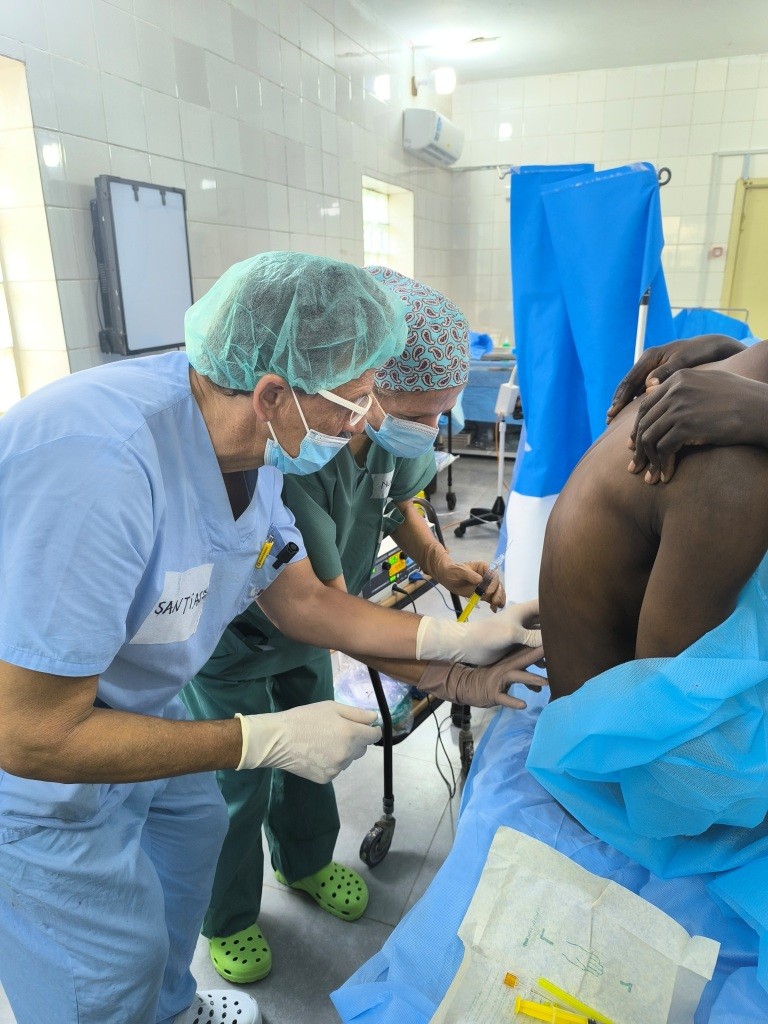
On one table, only spinal anaesthesia for hernias and 2 large lipomas were performed with local anaesthesia and sedation. It should be noted that on this table 3 caesarean sections were also performed by the hospital team, but with our collaboration in the spinal anaesthesia and monitoring. The pulse oximeter and the PANI were ours.
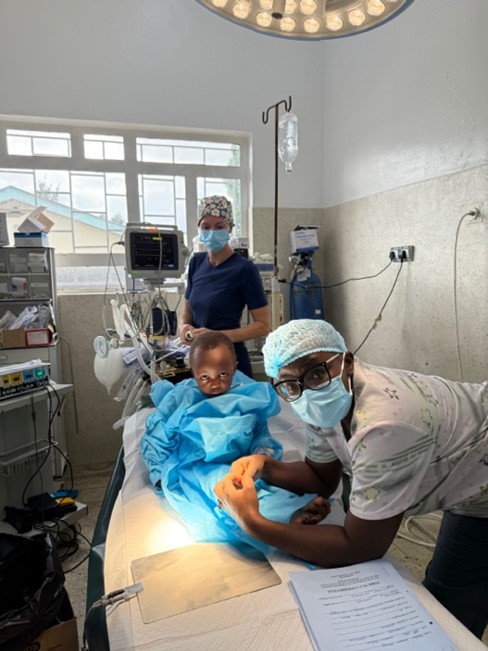
The third table combined adult rachis with paediatric general anaesthesia. For this purpose we mounted a Sevorane vaporiser connected to an oxygen bullet on one side and a Mapelson on the other. All children, except one 9 year old and one 10 year old who underwent a rachis with sedation, were done with laryngeal mask spontaneously, without complications. These patients only had a pulse oximeter for monitoring.
We set up a small ‘Awakening’ in the exit corridor for thyroidectomies and children.
We did not have any serious episodes of note.
We have left medication and material with the anaesthesia technician in charge, Benedicta. This 47 year old nurse is very well trained, very interested and helpful.
On the last day we didn’t have enough fentanyl and she got it for us from the pharmacy. I think that given the circumstances and knowing that you can get it there, you should not bring it from Spain.
The patients do NOT come to the operating theatre with a needle and the serums available there are mainly saline and Dextrose 5%. We managed to get several boxes of Ringer’s after protesting, but not enough.
Despite what it may seem, we worked well, comfortably and quite safely.
2.6. ASEPSIS AND SURGICAL SUPPLIES
They have an autoclave, and 2-3 people dedicated exclusively to the washing and sterilisation of material, which is very efficient, so except for the odd moment, we had no lack of material at any time.
2.7. OUR LIFE IN MAKURDI
We landed in Abuja on Saturday 10 May at 6am. We were held up at customs on arrival because of the equipment, which was quickly sorted out as soon as Dr Thaddeus arrived, which was delayed by about 1.5 hours.
We started the journey to Makurdi in 2 vans, one for the material and one for us, with a security guard. The trip is really uncomfortable, as the van is too small for the 13 people in it. It takes a little over 6 hours to reach Makurdi. There a big welcome awaits us with local songs and dances. They have also prepared a big welcome poster for us. Afterwards we have lunch in the hospital dining room and then we start unpacking the equipment to prepare the operating theatre for the next day..
Dr Thaddeus did the pre-selection of patients and prepared the surgeries for the 3 tables on the following days. The patient selection was very good, but not the planning, as he planned many goitre surgeries and few surgeries for children and adults with abdominal wall pathology, despite having made the indications beforehand. Fortunately, in the following days more patients appeared and we were able to complete a few days. We also found it somewhat difficult to make them understand that the order of the surgeries should be from the most complicated to the least complicated throughout the day, and not randomly as planned. In addition we found more complex patients in the last 2 days, so for future missions it would be good to warn that patients with hernias and giant goitres should be operated on the first days because of the complications that may arise.
On Sunday 11th, we were joined by Dr Salifou Hankouraou, a doctor with surgical training, who had travelled 3 long days from Niger. Salifou worked hard throughout the campaign, always trying to learn as much as possible with us.
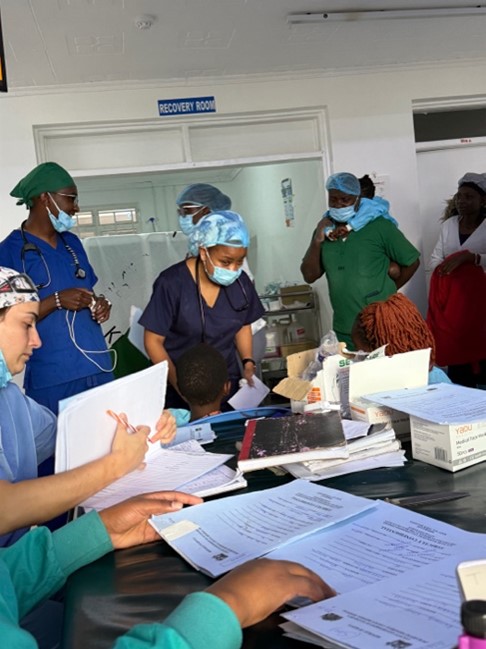
Every day we start with breakfast at 7:00 a.m. at the nursing home. We then travel to the hospital in two cars. Two or three members of the team handle the rounds and the corresponding discharges. Others are responsible for seeing patients undergoing surgery during the day and organizing the order of surgeries on the three operating tables.
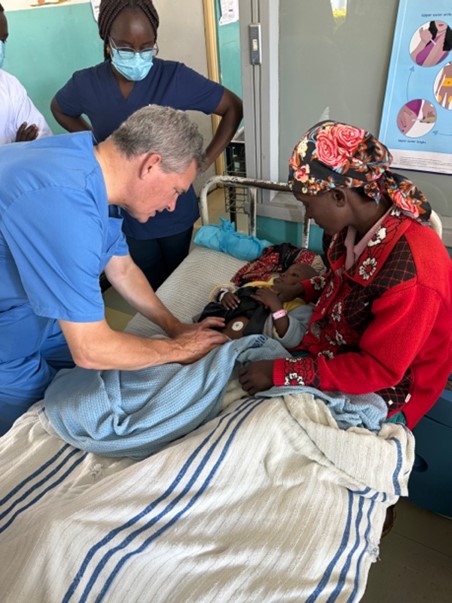
We operated like this without many incidents for five and a half days, stopping for lunch, finishing the shift between 9 and 11 p.m. Every day before leaving for the hotel, the team that finished first made a round of the rooms to check on the patients’ condition.
Lunch is prepared at the hospital, in a cafeteria in the office area. We ate very well and with a variety of food throughout the week. We have to thank the cook for the special gluten-free menu she prepared for Nuria and me every day.
Dinner is served at the residence, not as good or varied as the one at the hospital, but quite acceptable.
One evening, the Bishop of Makurdi, Wilfred Chikpa Anagbe, visited us. They hosted a large outdoor dinner, gave us each a gift, and we all ended up dancing.
On the last day, Friday the 16th, we operated on the remaining patients, collected everything we needed to take home, and before lunch, we were taken to a nearby market where we were able to buy some souvenirs.
We began the return trip, another nearly six hours to the Caritas residence in Abuja, where we stayed to catch the plane the next morning.
We returned home with very good feelings about this place and its people. Despite all the difficulties we encountered along the way, as always, it was worth it. Many thanks to all the extraordinary people who were part of this team of volunteers, for all the effort they put in with such humor and good vibes.
3. CONCLUSION
3.1 STRENGTHS OF THIS PLACE:
The hospital has a good infrastructure for this type of mission, with plenty of space and very cooperative staff. The donated materials are well cared for.
Dr. Thaddeus is cooperative and carefully selects patients. The entire staff is deeply involved in the campaign and is very pleasant and caring.
3.2. Improvement objetives:
Although patient selection was good, daily surgical planning needs to be improved to optimize time and resources.
More monitors should be obtained and a room adapted for general anesthesia recovery.
Undoubtedly, the biggest challenge for this campaign is obtaining visas, which has nothing to do with the destination hospital, but it is something to keep in mind when coordinating this mission. Above all, it is important to consider that it is almost essential to have someone on the team who can go to the embassy in person.
4. BUDGET:
4.1. COST PER PARTICIPANT:
Approximate cost per participant: €1.479,75 (± depending on the place of origin)
4.2. TOTAL COST OF THE CAMP:
Flight tickets Vigo/Gran Canaria/Granada-Madrid: €1,347.48
Flight tickets Madrid-Abuja: 9 flights: €8,632.56
Flight tickets Barcelona-Abuja: 2 flights: €2,159.68
Cancellation insurance: €449.46
Transportation Abuja-Makurdi round trip: €600
Visas: €2,838
Hotel Abuja: €250
TOTAL COST OF THE CAMP: €16.277,18
5. SIGNATURE
Signed: Ana María Gay Fernández
Team leader of the camp
Cirujanos en Acción